New Nailing System Used in Open Diaphyseal Fractures
Mohamed Abdel-AAl, Abdel-Aleem-Aziz Atallah and Abdel-Aleem M
DOI10.4172/2471-8416.100033
Mohamed Abdel-AAl1*, Abdel-Aleem-Aziz Atallah2 and Abdel-Aleem M2
1Department of Orthopedics, El-Barky General Hospital, Cairo, Egypt
2Department of Orthopedics surgery, Cairo, Egypt
- *Corresponding Author:
- Abdel-AAl MA
Department of Orthopedic, El-Bakry General Hospital, Cairo, Egypt
Fax: 1020995024
Tel: +20-02-26204528
E-mail: btmnail2010@hotmail.com
Received date: October 30, 2016; Accepted date: April 08, 2017; Published date: April 11, 2017
Citation: Abdel-AAI MA, Atallah AHAA, Sultan AAM (2016) New Nailing system used in Open Diaphyseal Fractures of Forearm in Adults. J Clin Exp Orthop 2:5. doi: 10.4172/2471-8416.100033
Copyright: © 2016 Abdel-AAI MA, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Introduction: Stabilization of open fractures is an important step in managing these injuries. Intratramedullary nailing of forearm fractures in adults is an acceptable and preferred method for internal fixation. In this study we tried to evaluate the functional end results of using a new nailing system in open diaphyseal fractures of forearm.
Patients and Method: Between May 2011 and February 2015 (45 months), Fifty-three patients (106 fractures) with open diaphyseal forearm fractures had been treated and followed using new intramedullary nailing technique (Be. Te. Radial & Ulnar Nails-Santam etal,) as a method of fixation and assessing their effectiveness clinically and radiologically. There were 17 females and 36 males. Their age ranged from 25 years to 45 years (mean 32 years).
Results: The final functional outcome was assessed utilizing Mayo Elbow Performance Score (MEPS) based on the parameters of pain, range of motions, stability and activities of daily life (ADL). The results of the study were: 25 (47.2%) Excellent, 20 (37.7%) Good, 6 (11.3%) Fair and 2(3.8%) Poor.
Conclusion: The use of intramedullary nailing in open diaphyseal forearm fractures in adults is recommended and may be alternative to plate osteosynthesis because of minimal surgical exposure, less scarring and disfigurement, lower risk of infection, lower risk of soft tissue injury, less risk of refracture after implant removal and minimal period of convalescence.
Keywords
Intramedullary nailing; Open forearm fractures
Introduction
Incidence of open fractures of forearm is higher than any other bone except the tibia. Bone union, restoration of limb functions and prevention of infection are the primary objectives in treatment of open fractures of extremities [1]. Intramedullary nailing has been used and proven in treatment of diaphyseal fractures of almost all long bones. The exception to this rule is in the forearm area, where plating is considered as the gold standard [2,3]. With open fractures, however this technique has many disadvantages including: large operative wound, needed for plate application which may add injury to already injured periosteal blood supply [4], difficult accessibility to proximal radius without risks of posterior interosseous nerve injury, refracture rate following plate extraction and high risk of infection compared to nailing techniquess [5,6]. Plating preference may be due to deficient rotational and linear stability of intramedullary nailing. This trend is currently changing, as newer types of locked nails evolved. This feature of medullary fixation that closely approximates the concept of "biological fixation" [7,8]. The aim of the present study evaluates the functional outcome of new interlocking nail system (Be. Te. Interlocking Nail System) in open diaphyseal forearm fractures in adults.
Patients and Methods
Twenty-Three adult patients (17 males) with open diaphyseal forearm fractures treated and followed between May 2009 and February 2012 (33 months). Fractures classified according to Gustilo and Anderson [8] classification Table 1.
| Sex/Fr. | G I | G II | G IIIA | G IIIB | Total |
|---|---|---|---|---|---|
| Male | 9 | 5 | 2 | 1 | 17 |
| Female | 4 | 2 | - | - | 6 |
| Total | 13 | 7 | 2 | 1 | 23 |
Table 1: Distribution of classification of fracture cases.
Exclusion criteria included patients less than 18 years, Monteggia or Galeazzi fractures, pathological fractures, refracture after previous surgery and associated skeletal, head, neurological or vascular injuries. Ages ranged between 25 and 45 years with mean age 31.5 years. All cases were operated upon within 24-72 hours following hospital admission.
Description of the study’s implants
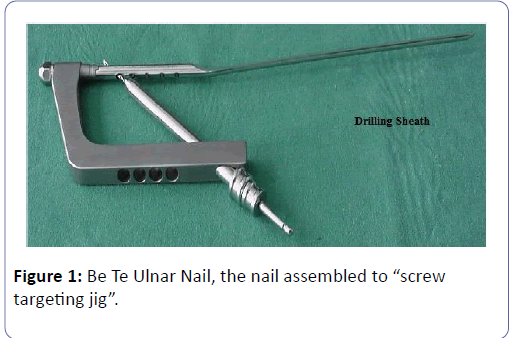
Ulnar Nail (Be Te Ulna Nail): It is anatomically shaped to fit the medullary canal. The distal part has triangular cross-section allowing automatic locking against rotational instability without further locking procedure. Nail tip is beveled to facilitate insertion. The proximal part is broader, rounded, angulated 3° posteriorly to fit natural widening and angulation of medullary cavity of proximal ulna and carries holes for proximal locking screws. The nail is not side- specific (Figure 1).
Radial Nail (Be Te Radial Nail): It is prebent, flexible and anatomically shaped fitting the medullary canal of radius according to three points fixation principle increasing to fivepoint fixation following the natural arcs of the medullary canal (Figure 2).
Nail tip is chamfered to facilitate its insertion. It reduces the radial fragments anatomically after proper insertion and tenses the interosseous membrane (an important step for restoration of normal range of prono-supination). The proximal end locks in subchondral bone of radial head and neck. Distally, the nail lies on the inside of opposite cortex and the distal end is curved to follow radial styloid contour. The nail is side- specific.
Operative Procedure
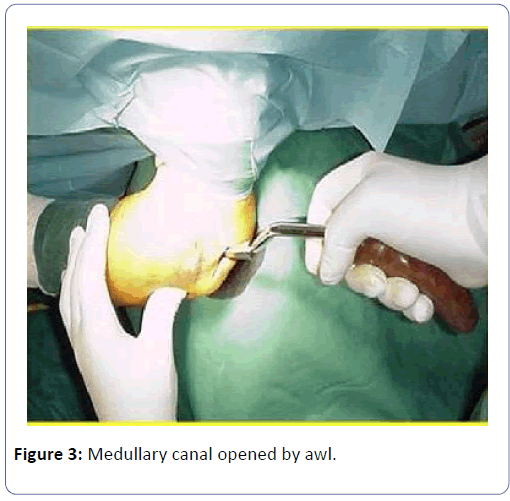
Under general or regional anesthesia, patient positioned supine on a table having a radiolucent arm board. The shoulder abducted and elbow flexed 90 degree for ulnar nailing whereas the arm extended for radial nailing. Meticulous debridement of wound layer by layer down to bone and copious irrigation with saline under pressure up to 5 liters solution used. Antegrade ulnar nailing done first, providing a stable forearm for retrograde nailing of radius. Entry point identified fluoroscopically at the most proximal point of olecranon and a small longitudinal incision about 1.5 cm made. Dissection carried down through subcutaneous tissue and triceps fascia. The canal opened using an awl (Figures 3).
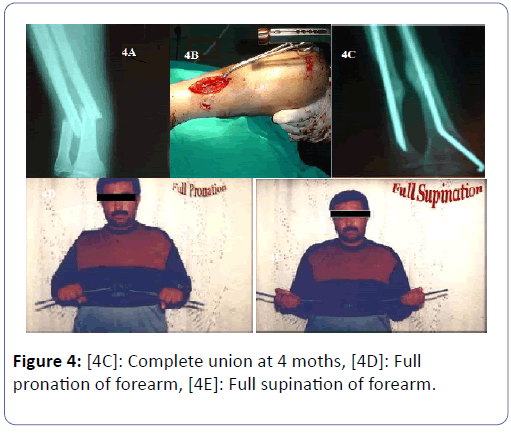
The nail inserted into the prepared bone hole with the targeting jig perpendicular to axis of rotation of elbow and insertion assisted by light mallet blows (Figure 4). Locking screws fixed in the cortical bone. One screw should be inserted towards the coronoid process which secured the nail against proximal migration. Screw targeting jig removed and an end-cap placed into the proximal nail end.
Radial nail length measured from the styloid process to subchondral bone of radial head. A short longitudinal incision done over the styloid radius and subcutaneous tissues dissected bluntly to avoid injury to superficial branches of radial nerve. The medullary canal opened with a curved awl. Selected nail fixed to "quick release insertion T-handle" Figure 2 and inserted into the prepared hole with the tip directed toward the opposite cortex. The quick release T-handle released 5-7 mm from the definitive position of nail and light blows done for full seating of nail. The distal end of nail left out of the medullary cavity to contour the radial styloid process. Postoperative care involved wound dressing every other day, a course of parentral antibiotic consisting of 3rd generation cephalosporin (1 gm/12 hours) (20 patients all GI and GII) and continued for one week. Combination of cephalosporin and aminoglycosides (80 mg gentamycin/8 hours) used in 3 patients (All GIII) and maintained for (10-15 days) but aminoglycosides stopped after one week and metronidazole (Flagyl) drip added to the regimen owing to suspicion of anaerobic infection. Patients were evaluated clinically weekly and radiographically at 4-weekly intervals till union and then at 3-monthly intervals.
Results
Patient-rated outcome assessed 1 year postoperatively, with use of Mayo Elbow Performance Score (MEPS) based on parameters of pain, range of motions, stability and activities of daily life (ADL) with 100 points scale. No cases of refracture developed. According to Mayo Elbow Performance Score (MEPS): 8 cases had excellent result (fall between 90-95 points), 10 cases had good result (fall between 78-88 points), 3 cases had fair result (fall between 62-73 points) and 2 cases had poor result (fall between 25-55 points).
No intraoperative complication that required change in operative procedure. Superficial infection developed in 3 cases (13%) while no cases of uncontrolled deep infection or bone infection (osteomyelitis). Eighteen patients (78.3%) were out of pain, four patients (17.4%) had mild to moderate pain and only one patient (4.3%) had severe pain. Total united cases were 22 cases (95.7%). Ninety cases united between 8-12 weeks, 3 cases united between 6-12 months without secondary intervention (bone grafting) and were considered delayed-union. One case of non-union treated with bone grafting and plating. Twenty patients (86.9%) attained full range of flexion/extension pronation/supination compared with the normal arm. Three patients showed limitation of 15-25ºC pronation and 20-25ºC supinations (compared to contralateral forearm). Out of 23 ulnar fractures, 21 ulnar nails removed (91.3%). Also, all radial nails were removed.
Discussion
Development of newer interlocking nail systems plus frustration of having to plate segmental forearm fractures and refracture after plate removal led to renewed interest in nailing of forearm fractures [9]. Newer studies are emerging which demonstrate comparable results to plate osteosynthesis after treatment with intramedullary nails [10,11]. WICK, et al. [11]. Reviewed 51 fractures treated by (True flex nail). The average time to healing after open fractures was 12.4 weeks. Two cases of pseudo-arthrosis observed (6.8%). No cases of refractures after nail extraction were observed. Weißer, et al. [12] reviewed the results in 32 patients after implanting 40 foresight nails. According to DASH (Disabilities of the Arm, Shoulder and Hand) score, excellent results achieved in 19 patients (86.4%). The time to radiological healing in 25 patients was between 3 and 6 months. Complications included: pseudo-arthrosis in one patient, delayed healing in two patients, incomplete synostosis in two patients and complete synostosis in one patient. Nail extraction was done in 13 patients (40%). No cases of refracture were seen. GAO, et al. [13] had reviewed the results in 18 patients treated with foresight nail. The average time of union for open fractures was 15 weeks. The average value of pronation and supination was 62° and 80°, respectively when compared with uninjured arm. Seven postoperative complications were seen (22%): one case of complete synostosis; two cases of retrograde migration of the locking screw (distal end of the ulnar nail) and four cases of superficial infection.
We achieved comparable results in our study. Meticulous debridement was an important step on dealing with these fractures. Copious irrigation was an essential tool but not a substitute for adequate debridement [3,6,8]. Five litres or more of saline used for wash with avoiding pushing contaminants into deeper tissues or up along medullary cavity. Antibiotic was not a substitute for proper and careful wound debridement. It continued for one week in 20 cases (all were GI and GII). It seem a reasonable time for these categories to avoid development of infection which coincident with many authors. Contrary, GIII required a longer period of antibiotic as soft tissue damage was more severe and liability of deep infection was highly anticipated [8].
Time to bony consolidation experienced in our patients did not differ from that after plate osteosynthesis [15,16] or other locked nailing [17,18]. The average time to bone healing was 16.2 weeks. There were three cases of prolonged healing and one case of non-union (4.3%). Compared with plate osteosynthesis, time to radiological union might seem long but restoration of extremity functions with the exception of heavy lifting and twisting was achieved in all patients (except one) by less than 16 weeks before radiographic consolidation. The rates of nonunion for both plate osteosynthesis and bundle nailing have been reported to be around 3% [19] which is comparable to our results (4.3%).
We observed full range of movement in 86.9% of patients; slight limitation of movement in 8.7% and severely restricted
Movement in 4.3% of patients, a result which is comparable to other studies. Nail extraction was not routinely performed. Candidates of nail removal were symptomatizing ones owing to subcutaneous position of distal end of radial nails and those who requested nail removal owing to psychological alertness. No further immobilization needed and the patient announced to avoid strenuous activities for 3 weeks at least.
Complications rate were low compared with other series with locked nailing probably because of strict exclusion of patients with vascular damage, refracture, pathologic fractures and less time delay between injury and surgery. Good results are also attributable to achievement of anatomical reduction in majority of cases along with allowance of early range of motions.
Despite all the advantages of intramedullary osteosynthesis, it must be stated that the learning curve associated with using the instruments is quite long.
Despite the total number of patients is small, it could be recommended that this implant might reduce non-union rates in open forearm fractures that following non-locked nails. Also, the results and complications are equivalent to that associated with plate osteosynthesis, and it can be considered as an alternative to plate fixation in open fractures of the forearm.
Conclusion
According to the results of our study, intramedullary nailing of diaphyseal forearm fractures undeniably affords comparable results with plating techniques with an added advantage, especially in segmental and comminuted fractures. The risk of refracture and the number of infectious complications appear to be low. Other advantages of nailing are the favorable cosmetics (due to insertion through micro-incisions). The chief shortcomings are exposure to radiation (minimized by upgrading of learning curve) and its slightly higher cost.
References
- Boyd HB, Lipinski SW, Wiley JH (1961) Observations on the non-union of the shafts of long bones. J Bone and Joint Surg. 43: 159-168.
- Dodge HS, Cady GW (1972) Treatment of fractures of radius and ulna with compression plates. J Bone and Joint Surg 54: 1167-1176.
- Ritmann W W, Schibli M, ligOwer M (1979) Open fractures. Long-Term Results in 200 cases. Clin Orthop and Related Research 138: 132-140.
- Rosacker JA, Kopta JA (1981) Both bones fractures of forearm: Review of surgical variables associated with union. Orthopedics 4: 1353-1356.
- Grace TG, Eversmann WW (1980) Forearm fractures treated by rigid internal fixation and early motion. J Bone and Joint Surg 62: 433-438.
- Langkamer VG, Ackroyd CE (1991) Internal fixation of forearm fractures in the1980s. Injury 22: 97-102.
- Weckbach A, Blattert TR, Weisser Ch (2006) Interlocking nailing of forearm fractures Arch. Orthop trauma surg 126: 309-315.
- Gustilo RB, Anderson JT (1976) Prevention of infection in the treatment of open fractures. J Bone and Joint Surg 58: 433-438.
- Richard RR, Corley FG, Rockwood CA, Green P, Bucho RW et al. (1976) Fractures of the shaft of radius and ulna. In:”Rockwood and Green’s Fractures in Adults”. edn 4 Philadelphia, Lippincott- Raven 1: 869-911.
- Bhandari M, Schemitsch EH, (2004) Fractures of the shaft of the ulna. J Orthop Trauma 18: 473-475.
- Myers GJC, Gibbons PJ, Glithero PR (2004) Nailing of diaphyseal forearm fractures. J Bone J Surg 86: 581-584.
- Wick M, Hahn PM, Müller EJ, Muhr G (1999) Intramedullary nailing of forearm fractures : The Trueflex Nail. Injury 30: 74-80.
- Weiber C, Weckbach A (2003) Interlocking nailing of forearm fractures with the ForeSight Nail: Oper Orthop. Traumatol 15: 151-169.
- Gao H, Luo CF, Zhang CQ, Zen BF (2005) Internal fixation of diaphyseal fractures of the forearm by interlocking intramedullary nail. J Orthop Trauma 19: 384-391.
- Mih AD, Coone WP, Idler RS, Lewallen DG (1994) Long-term follow-up of forearm bone diaphyseal plating. Clin. Orthop and Related Research 299: 256-258.
- Hertel R, Pisan M, Lambert S, Ballmer FT (1996) Plate osteosynthesis of diaphyseal fractures of the radius and ulna. Injury 27: 545-548.
- Holmenschlager F, Winckler S, Brug E (1995) Multifascicular intramedullary bundle nailing of the forearm. Rev Chir Orthop Reparatrice 81: 229-239.
- Jones DJ, Henley MB, Schemitsch EH, Tencer AF(1995) A biomechanical comparison of two methods of fixation of fractures of the forearm. J Orthop Trauma 9: 198-206.
- Weckbach A, Blattert TR, Weisser Ch (2006) Interlocking nailing of forearm fractures: Arch orthop trauma surg 126: 309-315.
- Goldfarb CA, Tull F, Ray D, Borrelli J (2005) Functional outcome after fracture of both bones of forearm. J Bone J Surg 87: 374-379.
- Visna P, Beitl E, Pilny J, Cizmar I, M. Valcha (2008) Interlocking Nailing of Forearm Fractures. Acta Chir Belg 108: 333-338.
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences