Osteoblastic cell adhesion on Strontium-incorporated porous nanostructured TiO2 coating prepared by micro-arc oxidation
Zhenxiang Zhang
DOI10.4172/2471-8416.100007
Zhenxiang Zhang*
Orthopedic Department, The Affiliated Taizhou people's Hospital of Nantong University
- *Corresponding Author:
- Zhenxiang Zhang
Orthopedic Department, The Affiliated Taizhou people's Hospital of Nantong University
Yingchun Road, Taizhou, Jiangsu 225300
People’s Republic of China
Tel: +86 21 86532798
E-mail: Kafeimao1982@126.com
Received date: November 04, 2015; Accepted date: November 04, 2015; Published date: December 21, 2015
Citation: Chen YP, Chen CY, Ke CJ, et al. Traumatic brain injury result in accelerated fracture healing: A Rat Model. J Clin Exp Orthop. 2015, 1:7. doi: 10.4172/2471-8416.100007
Copyright: © 2015 Chen YP, Chen CY, Ke CJ, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Objective: In the present work, strontium (Sr) was incorporated into TiO2 (Sr- TiO2) coatings on titanium by Micro-arc oxidation (MAO) technique in the Ca, P, Si-containing electrolyte to obtain the implant with good bioactivity. Methods: The surface topography, phase and element composition were characterized by scanning electron microscopy, X-ray diffraction and energy dispersive spectrometer, respectively. Osteoblast-like Mg63 cells were cultured on the surface of the coatings to evaluate their adhesion behavior. Results: Obtained results showed that compared with the Sr-free TiO2 coating, Sr was successfully incorporated, which did not alter its surface topography and phase composition. Adhesion cells on Sr-incorporated TiO2 coating was significantly enhanced compared with that on the Sr-free TiO2 coating. Conclusion: In conclusion, it is an interesting and promising way to regulate the functions of the coatings by introducing desired elements, such as Sr, by micro-arc oxidation technique.
Keywords
Micro-arc oxidation; Strontium; TiO2; Osteoblast; Adhesion
Introduction
Titanium and its alloys have been widely used as orthopedic implants because of their excellent biocompatibility and mechanical properties. An oxide layer, mainly TiO2, is spontaneously formed on the surface of titanium in air or the human body, which provides corrosion resistance [1,2]. However, TiO2 is not bioactive enough to form a direct bond with juxtaposed bone, which may translate into a lack of osteointegration that might lead to long-term implant failure [1,2].
Effects of trace elements on biological role have become an important topic in the research fields of bone formation and organism essential elements recently. The Strontium ion is involved in many metallo-enzymes and proteins including alkaline phosphatase (ALP) [3]. Depletion or supplementation of dietary Strontium has been shown to be responsible for variations in body weight, bone length and bone biomechanical properties [4], and the positive effect of Strontium on bone metabolism has been associated with growth hormone (GH) or insulin-like growth factor 1 (IGF-1) [4,5]. In vitro studies have also shown that Strontium is an essential trace element for promoting osteoblast cell adhesion, proliferation and differentiation, and inhibiting osteoclastic (bone resorbing) activity [4,6,7]. For these reasons, Strontium incorporated in bioactive glasses [8,9], calcium phosphates [10,11], or in other ceramics [12,13] have been investigated as potential materials to stimulate bone formation and inhibit bone resorption with promising results. However, Strontium-containing TiO2 ceramics or coatings have not been reported, and the effects of Strontium incorporation on the composition, microstructure and biological responses of TiO2 are not clear by now. Therefore, in this work, an interest has been taken in the preparation and characterization of Sr-containing TiO2 coating.
Micro-arc oxidation (MAO) is a plasma-assisted electrochemical method, which produces rough, thick and porous nanostructured oxide films on titanium [14,15]. Micro-arc oxidized films are hard and well-adhered onto metal substrate [14]. Besides, many bioactive ions can be incorporated into the micro-arc oxidized TiO2 coating by doping the electrolyte [14,15].In this work, porous nanostructured Sr-incorporated TiO2 coating (Sr-TiO2) was prepared by MAO in a novel Ca, P, Sr-containing electrolyte. Adhesion behavior of osteoblast-like MG63cells on the novel Sr- TiO2 coating is also discussed.
Materials and methods
Preparation of samples
Commercially pure Ti plates of 10 × 10 × 1 mm3 in size were used. The polished Ti plates were mechanically polished by SiC abrasive sandpapers. For TiO2 coating, the Ti plates were anodized in an electrolyte containing 0.05 mol/L glycerophosphate disodium solt pentahydrate (C3H7Na2O6P.5H2O, GP) and 0.1 mol/L Calcium acetate monohydrate [(CH3COO)2Ca.H2O,CA]. While for Sr- TiO2 coating, 0.04 mol/L Sr(CH3COO)2·2H2O was added into the electrolyte mentioned above. The current density, frequency, duty circle and duration time were fixed at 16.5 A/dm2, 800 Hz, 10% and 4 min, respectively. The schematic diagram of the experimental set up is shown in Figure 1. After MAO treatment, the samples were washed with deionized water and dried in air. The surface characterization of MAO-treated samples was performed by scanning electron microscopy (Philips XL30 FEGSEM) , X-ray diffraction (XRD, D/MAX-2550, Rigaku, Japan) and energy-dispersive X-ray spectrometry (EDS) attached to electron probe X-ray microanalysis system (EPMA, JAX-8100, Japan).
Cell culture
The mouse osteosarcoma cell line MG63 subclone 14 cells used in this work was purchased from Shanghai Chinese Academy of Science. MG63 cells were cultured in alpha MEM medium with glutamax (Gibco BRL) supplemented with 10% fetal calf serum (SCF, Eurobio) in a humidified atmosphere of 95% air-5% CO2 at 37°C. The culture medium was renewed every two days. When cells reached confluence, a trypsin-EDTA solution (0.5 g/L trypsin and 0.2 g/L EDTA, Gibco) was used to detach cells from the bottom of the culture flasks, and 1/3 of the total cells were transferred into a new tissue culture flask.
MTT assay
MTT assay was used to determine cell attachment. Cells were seeded at a concentration of 2 × 105 cells/cm2 onto the disks of Ti plates, TiO2 and Sr-TiO2 coatings. Cells were cultured on the disks for 1, 5, 10 and 24 hours, respectively, in a 37°C incubator with 5% CO2. At the pre-determined time points, each disk was transferred to wells of a new 24-well plate and 1.5 ml of medium was added to each disk. One hundred and fifty microliters of freshly prepared 5 mg/ml MTT was added to each well containing the disks. The plates were placed in an incubator at 37°C for 3 h. The supernatant of each well was removed and acidified isopropanol (0.04 M HCl in isopropanol) was added to all wells and mixed thoroughly to dissolve the dark-blue crystals. The absorbance was measured with a spectrophotometer at a wavelength of 570 nm with a subtraction of the absorbance at 650 nm. Cell number was determined using a linear correlation between absorbance and MG63 cell concentration.
Fluorescence staining
MG63 cells were seeded on Sr-TiO2 coatings, TiO2 coatings and Ti plates in 24-well plates at a seeding density of 1 × 104/cm2 cells well-1. After culturing for 5 and 10 h, acridine orange staining was used to directly count the cells. In brief, samples for acridine orange staining were ? xed in 95% ethanol for 15 min. After air drying, samples were stained in 0.1 mg/ml acridine orange (Sigma, USA) for 2 min. After rinsing with PBS, the samples were observed under a ?uorescence microscope.
Cell morphology
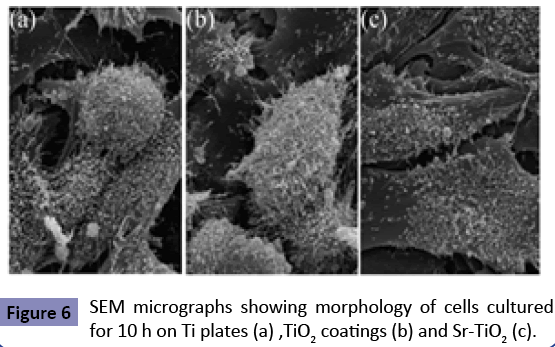
Cells were seeded on Ti plates, TiO2 and Sr-TiO2 coatings at a density of 1 × 104/cm2 in alpha MEM supplemented with 10% PBS and were cultured under standard cell culture condition for 10 h. The samples then were washed with Phosphate buffer saline (PBS) and double-distilled water respectively, and fixed with 2.5% glutaraldehyde buffered by PBS. Then the samples were dehydrated in a graded series of alcohol (50%, 70%, 90% and 100%) and amyl acetate following critical-point drying. The morphology of the adhered cells was observed using SEM.
Actin cytoskeleton
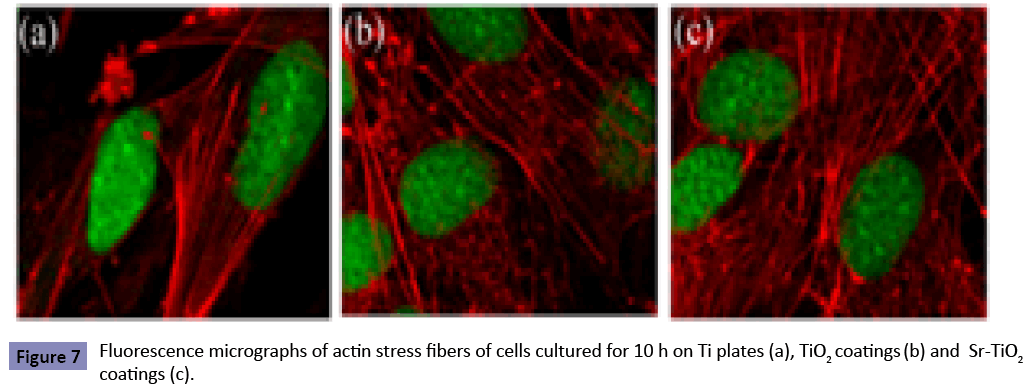
Each material was incubated with 1 × 104 cells. Cells adherent to the disks for 10 h were fixed by incubation in 3.7% formaldehyde dissolved in PBS for 10 min at room temperature. The disks were washed three times with PBS and treated with 1% Triton X-100 in PBS for 5 min to permeate the cell membranes. After being rinsed gently with PBS, the disks were blocked for 10 min with 1% heat-denatured bovine serum albumin (prepared by heating at 80°C for 5 min), and the actin cytoskeleton was subsequently labeled by incubation to FITC-phalloidin(Sigma) for 40 min at 37°C. Then the disks were rinsed in PBS for three times. Samples were examined with a microscope Olympus BX 51 equipped with epifluorescence (Olympus, France).
Statistical analysis
One way ANOVA and Tukey’s multiple comparison tests were performed to detect significant (p ≤ 0.05) effects of the experimental variables. Results were analyzed using Student’s t test with a sample numbers of at least four samples. Error bars represent mean ± standard deviation. The level of significance was set at p=0.05.
Results
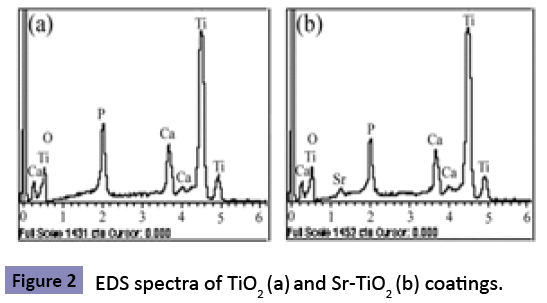
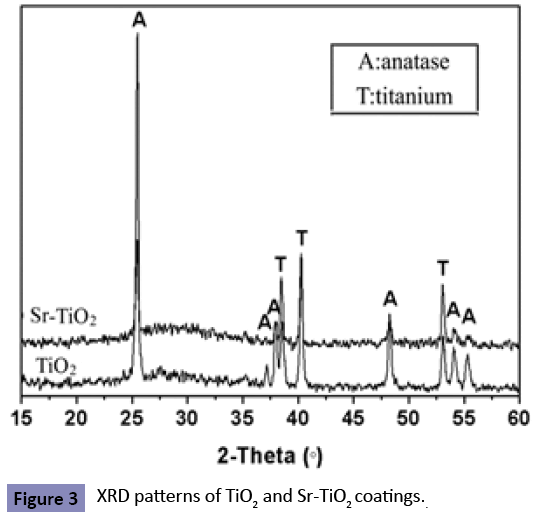
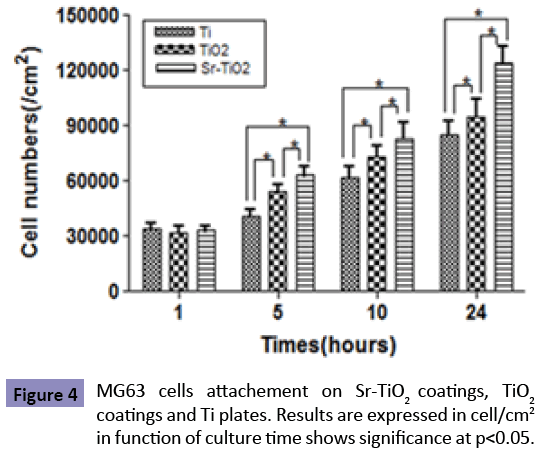
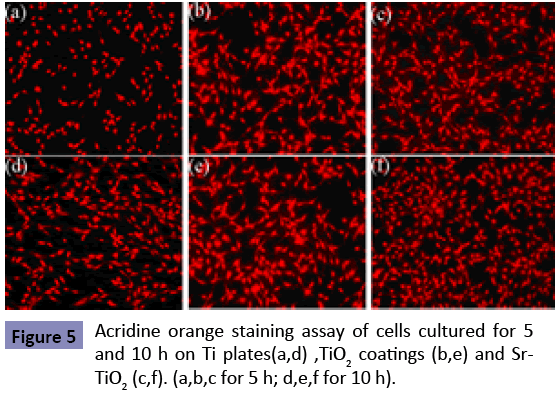
The surface morphologies of TiO2 and Sr-TiO2 coatings at low magni?cation (2000X) are shown in Figures 2 (a,b). It can be investigated that both samples are porous with pore size about 3-5 μm. These pores are well separated and homogeneously distributed over the coating surfaces. Figures 2 (c,d) show the surface morphologies of TiO2 and Sr-TiO2 coatings at higher magni?cation (50,000X), respectively. It is observed that at a higher magni?cation, both the coating are fully covered by the nano-grains with the size about 30-50 nm. No obvious differences in morphology are observed between TiO2 and Sr-TiO2 coatings Figure 3 shows the element compositions of the micro-arc oxidized coatings determined by ED’s spectrum. Compared with the EDS spectrum of TiO2 coating (Figure 3a), a obviously feature peak of Sr was clearly observed in that of Sr-TiO2 coating (Figure 3b), indicating that Sr was successfully introduced into the coating. The XRD patterns of the TiO2 and Sr-TiO2 coating are displayed in Figure 4. Only anatase phase was detected in both micro-arc oxidized coatings, indicating that the phase composition of the TiO2 coating was not altered apparently after the incorporation of Sr. Figure 5 shows the MTT result of the cells cultured on Ti plates, TiO2 and Sr-TiO2 coatings for 1, 5, 10 and 24 h. During the incubation of first 1 h after the cell plating, most of cells attached onto each substrate, and no significant difference was observed (p>0.05). The result of MTT assay indicated a quicker increase in cell quantity on Sr-TiO2 coatings when compared with Ti plates and TiO2 coatings. At 5, 10 and 24 h, it was observed that the cell quantity on TiO2 coatings was more than that on Ti plates (p<0.05), but less than that on Sr-TiO2 coatings (p<0.05). Therefore, Sr-TiO2 coatings surface could be more favorable for the attachment of osteoblasts. The attachment of MG63 cells on the Sr-TiO2 coatings, TiO2 coatings and Ti plates is also directly characterized by acridine orange staining assay on hour 5 and 10 after cell seeding (Figure 6). Within the first 5 h of culture, the visible cells number on the Sr-TiO2 coatings, TiO2 coatings and Ti plates kept increasing, indicating that cells attach on these three types of substrates. However, MG63 cells apparently attach faster on the Sr-TiO2 coatings, as shown by the markedly higher osteoblastic number on hours 5 and 10. Figure 7 shows osteoblastic morphology on three substrates. It can be detected that MG63 cells cultured on the Sr-TiO2 coatings, TiO2 coatings and Ti plates for 10 h show different morphologies. Apparently, after seeded on Sr-TiO2 coatings for 10 h, cells display more spread-out morphology, highly connecting with the surface, when compared with that on TiO2 coatings and Ti plates. Fluorescence micrographs of actin stress fibers in the cells on all the three substrates after incubation 10 h are shown by Figure 8. After 10 h of incubation, osteoblasts on Ti plate exhibited the weak formation of actin fibers within their cytoplasm. Conversely, well-defined actin stress fibers distributed through the body of cells cultured on TiO2 and Sr-TiO2 coatings. With the stronger actin cytoskeleton in cells adhering to Sr-TiO2 coating, the cells are stiffer and resist detaching shear forces acting on them more efficiently.
Discussion
Adhesion belongs to the first phase of cell/material interaction and the quality of this stage influences the capacity of cells to proliferate and differentiate itself on contact with the implant. Surface chemistry and topography play an important role in cell adhesion on biomaterial [15,21]. In this work, MAO technique is used to create a porous nanostructured Sr-containing TiO2 coating on Ti plate. The initial adhesion of osteoblast-like MG63 cells on the modified Ti plates, as well as its possible signal transduction pathway, is evaluated. The term “attachment” in the biomaterial domain occurs rapidly and involves short-term events like physico-chemical linkages between cells and materials involving ionic forces, van der Walls forces, etc. [15]. The importance of cell-substratum attachment for cellular proliferation and differentiation is widely recognized [15,17,18,20,21]. In this work, the highest number of MG63 osteoblastic cells attach on Sr-TiO2 coating, and the number of cells attached on Ti plates is lowest (shown as Figure 5). This phenomenon indicates that attachment of MG63 cells on Sr-TiO2 coating is superior to that on Ti plate and TiO2 coating. Surface chemistry of the biomaterials can greatly influence the cell attachment [16,18]. It has been reported that Sr can increase the activity of 1α,25-dihydroxyvitamin D3- dependent promoters in osteoblasts, which is well known to play a critical role in calcium and phosphate homeostasis across the cell membrane [22,23]. Therefore, it is possible that the Sr released from Sr-TiO2 coating may contribute to extracellular pH changes by influencing Ca2+-H+ exchange across the cell membrane, causing the structural alteration of the cell transmembrane proteins (such as integrins). The altered transmembrane proteins may easily interact and bond with proteins adsorbed on the Sr-TiO2 coatings from the culture medium, promoting the attachment of MG63 cells onto the surface. Surface topography is another factor that plays an important role in cell attachment [15,20,21]. Although a comparison of various studies revealed few consistent trends in the effects of surface topography on initial cell attachment [15], the most commonly observed trends are that porous structure is beneficial to osteoblastic attachment [24,25]. The porous Sr-TiO2 coating can facilitate the adsorption of proteins in the culture medium by providing a larger contact area at sample-medium interface, which are favorable for promoting the osteoblastic MG63 cell attachment. Spreading on biomaterial is an important step for essential biological properties of osteoblasts [15]. Surface chemistry of the biomaterials can significantly influence the osteoblastic spreading [16,18]. It has been reported that incorporating Sr into HA coating could promote the spreading of osteoblast [26]. Zhu et al. also demonstrated that osteoblasts were significantly more flatten on Sr-containing coating [27]. In this present work, we have observed that after seeded on Sr- TiO2 coatings for 10 h, cells display more spread-out morphology, highly connecting with the surface, when compared with that on TiO2 coatings and Ti plates (as shown by Figure 7). The Sr released from Sr-TiO2 coating could bind with oxygen, forming a Sr network structure on the surface, which is capable of holding elements of the proteins together in an organised fashion, thus contributing to the architecture of connective tissue. It is possible that these proteins are adsorbed onto the bound Sr network, promoting better osteoblastic spreading via interaction with the integrins on MG63 cells and, in turn, triggering certain specific signals, which could have a stimulatory effect on the bone mineralization process [6,7,28]. This possibility is supported by our findings that MG63 cells display more mature cytoskeleton organisat?ion on Sr-TiO2 coatings when compared to the polished Ti plates and TiO2 coatings (as shown by Figure 8). However, the precise mechanism by which Sr affects osteoblastic spreading should be further investigated. Surface topography is another factor playing an essential role in osteoblastic spreading [15,19-21]. Some researchers have stated that bone cells spreaded more flatten on nanostrucured porous coatings as compared to rough ones [15]. On the other hand, contrary conclusions bave been induced by other researchers [20,21]. A simple conclusion will be difficult to be executed for the relationship between the surface topography and osteoblastic spreading. In the present work, we investigate that the spreading of MG63 cells cultured on porous TiO2 and Sr-TiO2 coatings for 10 h is more pronounced when compared to that on polished Ti plates (shown as Figure 6), suggesting that spreading is promoted by the surrounding porous nanostructures.
Conclusion
In this work, Sr was successfully incorporated into porous nanostructured TiO2 coating by the MAO technique, and surface characteristics of the Sr-containing TiO2 coating, such as phase composition, as well as the porous nanostructure, were not altered apparently as compared to Sr-free TiO2 coating. In vitro experimental evidences were reported that the Sr-TiO2 coating was advantageous to MG63 cell adhesion.
Acknowledgment
This work was supported by Natural Science Foundation of China (81401770).
References
- Hayashi M, Jimbo R, Lindh L, SotresJ (2012)In vitro characterization and osteoblast responses to nanostructured photocatalytic TiO2 coated surfaces. Acta Biomater 8:2411-2416.
- Nagai A (2012)Response of osteoblast-like MG63 cells to TiO2 layer prepared by micro-arc oxidation and electric polarization. J Eur Ceram Soc32:2647-2652.
- Bakker AD, Zandieh-Doulabi B, Klein-Nulend J (2013)Strontium Ranelate affects signaling from mechanically-stimulated osteocytes towards osteoclasts and osteoblasts. Bone 53:112-119.
- Saidak Z, Marie PJ (2012)Strontium signaling: Molecular mechanisms and therapeutic implications in osteoporosis. PharmacolTher136:216-226.
- Li Y, Li J, Zhu S, Luo E (2012)Effects of strontium on proliferation and differentiation of rat bone marrow mesenchymal stem cells. Biochem Bioph Res Co418: 725-730.
- Caverzasio J (2008)Strontium ranelate promotes osteoblastic cell replication through at least two different mechanisms. Bone42:1131-1136.
- Römer P, Desaga B, Proff P, Faltermeier A (2012)Strontium promotes cell proliferation and suppresses IL-6 expression in human PDL cells Ann Anat194:208-211.
- Gentleman E, Fredholm YC, Jell G, Lotfibakhshaiesh N (2010)The effects of strontium-substituted bioactive glasses on osteoblasts and osteoclasts in vitro. Biomaterials31:3949-3956.
- Wu C, Zhou Y, Lin C, Chang J (2012)Strontium-containing mesoporous bioactive glass scaffolds with improved osteogenic/cementogenic differentiation of periodontal ligament cells for periodontal tissue engineering. ActaBiomater8:3805-3815.
- Yang L, Perez-Amodio S, Barrère-de Groot FY, Everts V (2010)The effects of inorganic additives to calcium phosphate on invitro behavior of osteoblasts and osteoclasts. Biomaterials31:2976-2989.
- Schumacher M, Lode A, Helth A, Gelinsky M (2013 )A novel strontium(II)-modified calcium phosphate bone cement stimulates hMSC proliferation and osteogenic differentiation in vitro. ActaBiomater.
- Schumacher M, Lode A, Helth A, Gelinsky M (2012)Antibacterial and biological characteristics of silver containing and strontium doped plasma sprayed hydroxyapatite coatings. ActaBiomaterialia8:3144-3152.
- Fielding GA, Roy M, Bandyopadhyay A, Bose S (2007)Preparation and cell-materials interactions of plasma sprayed strontium-containing hydroxyapatite coating. Surface and Coatings Technology201:4685-4693.
- Zhao BH (2013)Effect of Zn content on cytoactivity and bacteriostasis of micro-arc oxidation coatings on pure titanium. Surface and Coatings Technology228:428-432.
- Anselme K (2000) Osteoblast adhesion on biomaterials. Biomaterials21:667-681.
- Felgueiras HP, Evans MD, Migonney V (2015) Contribution of fibronectin and vitronectin to the adhesion and morphology of MC3T3-E1 osteoblastic cells topoly(NaSS) grafted Ti6Al4V. ActaBiomater 28:225-233.
- Minagar S, Li Y, Berndt CC, Wen C (2015)The influence of titania-zirconia-zirconium titanate nanotube characteristics on osteoblast cell adhesion.ActaBiomater12:281-289.
- Frandsen CJ, Noh K, Brammer KS, Johnston G, Jin S (2013) Hybrid micro/nano-topography of a TiO2 nanotube- coated commercial zirconia femoral knee implant promotesbone cell adhesion in vitro. Mater SciEng C Mater BiolAppl 33:2752-2756.
- Brun P, Scorzeto M, Vassanelli S, Castagliuolo I (2013) Mechanisms underlying the attachment and spreading of human osteoblasts:from transient interactions to focaladhesions on vitronectin-grafted bioactive surfaces. ActaBiomater 9:6105-6115.
- Webster TJ, Siegel RW, Bizios R (1999)Osteoblast adhesion on nanophase ceramics. Biomaterials20: 1221-1227.
- Bodhak S, Bose S, Kinsel WC, Bandyopadhyay A (2012)Investigation of in vitro bone celladhesion and proliferation on Ti using direct current stimulation. Mater SciEng C Mater Biol Appl 32:2163-2168.
- Zhu LL, Zaidi S, Peng Y, Zhou H (2007)Induction of a program gene expression during osteoblast differentiation with strontium ranelate. Biochemical and Biophysical Research Communications355: 307-311.
- Chattopadhyay N (2007)The calcium-sensing receptor (CaR) is involved in strontium ranelate-induced osteoblast proliferation. Biochemical Pharmacology74: 438-447.
- Karlsson M (2003)Initial in vitro interaction of osteoblasts with nano-porous alumina Biomaterials24:3039-3046.
- Chen J (2010)Osteoblast-like cell ingrowth, adhesion and proliferation on porous Ti-6Al-4V with particulate and fiber scaffolds Materials Science and Engineering:C30:647-656.
- Boanini E, Torricelli P, Sima F (2008)Strontium-substituted hydroxyapatite coatings synthesized by pulsed-laser deposition: In vitro osteoblast and osteoclast responseActaBiomaterialia4:1885-1893.
- Zhu Y, Zhu M, He X, Zhang J, Tao C(2013) Substitutions of strontium in mesoporous calcium silicate and their physicochemical and biological propertiesActaBiomaterialia9:6723-6731.
- Zhang W, Shen Y, Pan H, Lin K (2011) Effects of strontium in modified biomaterials. ActaBiomaterialia7:800-808.
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences