Prospective Study on Functional Outcome of Retrograde Femoral Nailing in Distal Third Femoral Fractures
Prasanna Anaberu, Madhan Jeyaraman*, Kartavya Chaudhari, Ajay SS, Sabarish K and Preethi Selvaraj
Prasanna Anaberu1, Madhan Jeyaraman1*, Kartavya Chaudhari1, Ajay SS1, Sabarish K1 and Preethi Selvaraj2
1Department of Orthopedics, JJM Medical College, Davangere, Karnataka, India
2Department of Community Medicine, SSSMCRI, Kancheepuram, India
- *Corresponding Author:
- Madhan Jeyaraman
Department of Orthopaedics
JJM Medical College
Davangere, Karnataka, India
Tel: +918310600785
E-mail: madhanjeyaraman@gmail.com
Received date: March 22, 2019; Accepted date: April 15, 2019; Published date: April 23, 2019
Citation: Prasanna A, Jeyaraman M, Chaudhari K, Ajay SS, Sabarish K, et al. (2019) Prospective Study on Functional Outcome of Retrograde Femoral Nailing in Distal Third Femoral Fractures. J Clin Exp Orthop Vol.5 No2:65. DOI: 10.36648/2471-8416.5.2.65
Copyright: © 2019 Prasanna A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: Due to the rapid industrialization, modern lifestyle and the fast pace of life, there is a concomitant rise in a road traffic accident that cripples many lives of the general population. The distal 1/3rd femoral fractures constitute 6% of all femoral fractures. These fractures pose a great challenge in management due to the involvement of soft tissue injury, intra-articular extension, and injury to the extensor mechanism. The debates on the choice of implant for distal femoral fractures are on-going among orthopedic surgeons. Controversy still remains regarding the optimum device for distal femur fixation.
Objectives: To evaluate and compare the clinical and the radiological outcomes of distal 1/3rd femoral fractures stabilization using retrograde nailing constructs.
Materials and Methods: After the screening of patients, a total of 113 cases, who were enrolled in the study, were subjected for surgical management of distal 1/3rd femur fractures with retrograde femoral nailing. All the patients were followed up clinically and radiologically at the immediate post-op period and at the end of 1, 3, 6, 12 and 18 months. The efficacy and functional outcome of distal femoral retrograded nailing were charted according to Lysholm knee scores. All cases were followed up for complications and were treated accordingly.
Results: In our study, 113 cases underwent surgical management with distal femoral retrograde nailing. The results were analyzed according to Lysholm’s knee scoring showed excellent in 55 cases (48.67%), good in 39 cases (34.51%), fair in 11 cases (9.73%) and poor in 8 cases (7.07%). The correlation analysis with Pearson’s correlation coefficient (r) was 0.8 which show a highly positive correlation between the union of distal femoral fracture and retrograde distal femoral nailing.
Conclusion: Retrograde distal femoral nailing for AO/ASIF type A and type C distal femoral fractures are a proven and reliable method of fixation. This safe, successful, effective, reliable and useful technique should find a place in the armamentarium of every orthopedic surgeon dealing with distal femoral fractures that initially requires attention to details of the technique to prevent complication and to improve the functional quality of life.
Keywords
Distal femoral fractures; Retrograde nail; Lysholm knee Score; Locking compression plate
Introduction
In recent years, due to the rapid industrialization, modern lifestyle and fast pace of life had led to a concomitant rise in a road traffic accident that cripples many lives, life expectancy, old age population, dangers of osteoporosis and fractures. The incidences of distal femoral fractures are 37 per 1 lakh personyears. The distal 1/3rd femoral fractures constitute 6% of all femoral fractures [1]. These fractures occur in bi-modal distribution as high energy trauma in younger age group and low energy fractures due to osteoporosis in the elder age group. Due to extensive comminution, soft tissue damage, an extension of the fracture into the knee joint, neurovascular damage and injury to the extensor mechanism in the distal femur, these distal femur injuries were complicated and difficult to manage [2].
The orthodox management of distal third femur fractures described by Watson Jones and John Charnley comprised of skeletal traction, manipulation of fracture and external immobilization in the form of casts and braces. This method was associated with deformity, shortening, fibrous ankylosis of the knee, knee joint incongruity, malunion, quadriceps wasting, knee instability, and early knee osteoarthritis. The dissatisfaction with these treatment methods led to the development of newer techniques of fracture management. The distal femoral fractures are best treated with open/closed reduction and surgical stabilization with load sharing or load-bearing implants [3].
The osteosynthesis in the distal femur could be difficult because of the thin cortex, comminution, osteopenia, complex injuries associated soft tissue injuries, a distal wide medullary canal and involvement of the knee joint. Most surgeons agree that distal femoral fractures need to be treated operatively to achieve optimal outcomes. The debate continues around the choice of implant for fixation of metaphyseal-diaphyseal fractures. The type of device depends on variables, fracture personality, and soft tissues. The current method of open reduction and internal fixation has become evident in the recent years with good results being obtained with the AO blade plate, dynamic condylar screw, intramedullary supracondylar nail and locking compression plate [4,5].
After thorough meta-analysis research, the technique of retrograde intramedullary nailing was the most ideal for distal 1/3rd femoral fractures. The intramedullary nailing act as a load sharing device which gives good results with minimal soft tissue dissection and good stability. The advantage of an intramedullary device is that it aligns the femoral shaft with condyles reducing the tendency to place various movements at the fracture site. The reduced bending movement of an intramedullary device has substantially reduced failure of fixation in osteoporotic bone [6]. Intramedullary nails offer potential biomechanical advantages over plates and screws because their intramedullary location results in less stress on the implant, they have the potential for load sharing and can be inserted with minimal stripping of soft tissue. The retrograde intramedullary distal femoral nail has the advantages of fracture hematoma preservation, reduced blood loss, minimal soft tissue damage, less operative time and reduced rate of infection. Controversy still remains regarding the optimum device for distal femur fixation [7].
Objectives
To evaluate and compare the clinical and the radiological outcomes of distal 1/3rd femoral fractures stabilization using retrograde nailing constructs.
Materials and Methods
• Health care setup-Tertiary Care Hospital
• Setting-Bapuji Hospital and Chigateri Government General Hospital, JJM Medical College, Davangere, Karnataka
• Duration of the study-2012 to 2017
• Type of the study-Prospective cohort study
• Level of evidence-Level IV
• Sample size-147
• Sampling technique-Convenient sampling
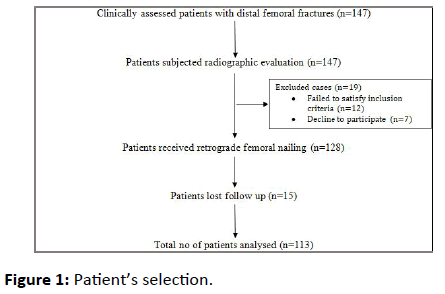
• Selection of cases-Among 147 clinically and radiologically confirmed distal femoral fracture cases, 12 cases failed to satisfy the inclusion criteria and 7 cases declined to participate in the study. The remaining 128 cases underwent surgical management as per our study protocol. A total of 15 cases lost to follow up in our study period. Hence 113 cases were taken into consideration for statistical analysis
• Radiological assessment-Anteroposterior and lateral views of full-length femur and knee were done
• Functional assessment-Lysholm knee scoring for retrograde distal femoral nailing. Osseous healing was defined as the radiographic presence of bridging callus formation and crossing trabeculae on AP and lateral radiographs at least three healed cortices. Clinical healing was defined as the absence of functional pain and local tenderness at the previous fracture site
• Follow up-Clinical and radiological analysis at the immediate post-op period and at the end of 1, 3, 6, 12 and 18 months. Patient’s selection flow chart in Figure 1
Inclusion criteria
• Patients with age between 20 to 70 years of age
• Patients with clinically and radiologically confirmed distal 1/3rd femoral fractures of AO types A1, A2, A3, C1, and C2
• Patients with type 1, 2, 3a and 3b compound fractures according to Gustilo Anderson classification for open fractures
• Patients who are medically fit for surgery
• Patients who have given written consent for treatment as per our protocol
Exclusion criteria
• Patients with age less than 20 and more than 70 years of age
• Patients with proximal 1/3rd and middle 1/3rd femoral fractures
• Patients with distal 1/3rd femoral fractures of AO types B and C3
• Patients with type 3C compound femoral fractures according to Gustilo Anderson classification for open fractures
• Patients with pathological distal 1/3rd femoral fractures
• A patient who are medically unfit for surgery
• A patient who has not given written consent for treatment as per our protocol
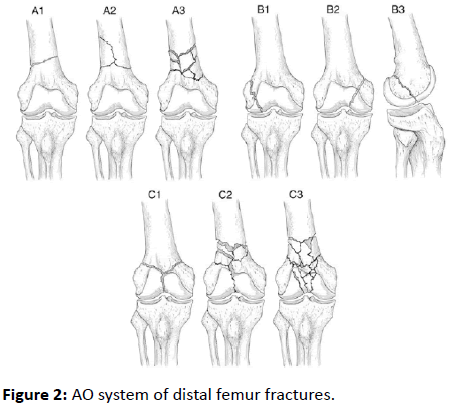
After getting IEC and informed and written consent from the patient’s attendees, the patients enrolled in the study were subjected for thorough clinical examination. The baseline investigations and radiographic analysis of the affected femur were analyzed. According to Gustilo and Anderson classification of open fractures, the compound fractures were treated with wound debridement and IV antibiotics in view to control any infection. All the cases were posted for surgical management with distal femoral nailing and follow up according to our study protocol. The other associated injuries were addressed off with appropriate management (Figure 2).
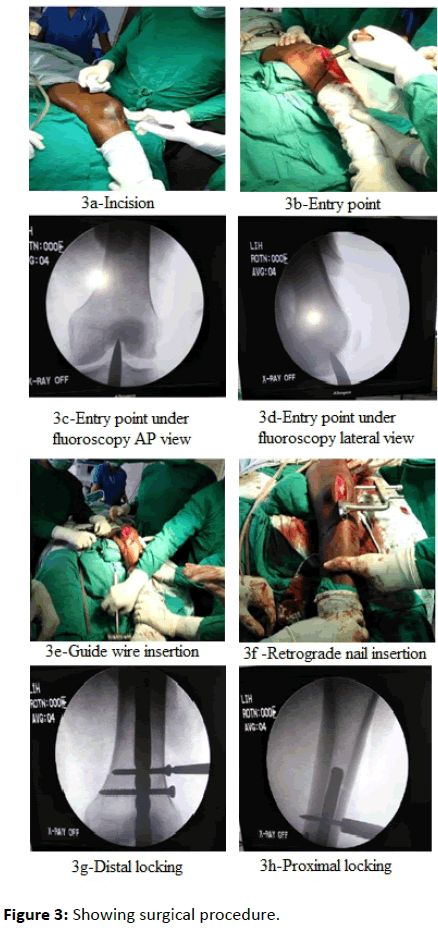
The surgical procedure of intramedullary retrograde distal femoral nailing system
Pre-operative planning: The nail diameter was determined the level of the isthmus by measuring the diameter of the femur on an AP X-ray (Figure 3).
Operative technique:
Anaesthesia: All the patients were operated under either spinal anesthesia or epidural anesthesia.
Reduction of fracture: The patients were placed in supine with the knee flexed to 30°-60° and closed reduction of the fracture was done by the traction and internal rotation which was confirmed by the fluoroscopic guidance.
Preparation: The patients were scrubbed, prepared and draped. Prophylactic IV antibiotic and tetanus toxoid were given in all patients 30 mins before surgery.
Approach: Make a longitudinal 2 cm skin incision, just distal to the inferior patellar pole, over the midline of the patellar tendon. Spread the medial parapatellar soft tissues longitudinally and retract (or split) the patellar tendon gently to allow for guide-wire insertion.
Entry point and insertion of guide wire: The entry point for the nail was in line with the axis of the medullary canal, just below the crest of the intercondylar notch. With the bone awl, PCL was identified and 1 cm anterior to it, entry was taken that is confirmed under C-arm guidance. Under C-arm guidance, the guide wire was inserted into the medullary canal through the entry point taken, respecting a 7-degree valgus angle to the horizontal plane of the joint.
Reaming: Using the cannulated reamer in an increment of 0.5 mm each, the reaming of the medullary cavity was done for about 0.5-1 mm more than the planned nail diameter.
Insertion of the retrograde distal femoral nail: After confirming satisfactory fracture reduction, an appropriate size nail as determined preoperatively was assembled to insertion handle and inserted manually by slight twisting movements of the hand. The nail was passed so as its end is just proximal and buried under the chondral surface.
Locking of the nail: Distal locking was usually performed first and then followed by the proximal locking, which allows the surgeon for the proper alignment of fracture fragments and the position was confirmed with an image intensifier.
Closure: The surgical closure was done in layers and the sterile dressing applied over wound and compression bandage was given.
Post-operative protocol: Intravenous antibiotics were given for 5 days followed by oral antibiotics for 5 days. Injection Zolendronic acid infusion was administered to improve the degree of osteoporosis. The active and passive exercises were initiated within 48 hours of surgery. Partial weight bearing was allowed on the 5th postoperative day.
Follow up: Tablet Risedronate 35 mg once weekly for 12 weeks were given to improve the bone mineral density in patients with severe degree osteoporosis. All the patients were advised to completely weight bearing after 10-12 weeks of the post-operative period. All patients were followed up at the end of 1, 3, 6, 12 and 18 months. At each follow-up, the radiographs of full-length femur were taken to assess the fracture union and the complications. The functional results were calculated according to the Lysholm score.
Implant removal: All patients enrolled in the study were offered with surgical implant removal at an average of 26 months post-surgical procedure who showed the clinical and the radiological union of fractures and improved functional quality of life.
Results
A total of 128 cases were enrolled in the study that was divided into two groups and the surgical treatments were instituted as per our study protocol. A total of 15 cases lost to follow up post procedure. Hence 113 cases were taken into consideration for statistical analysis. The descriptive statistics were reported as mean (SD) for continuous variables, frequencies (percentage) for categorical variables. Data were statistically evaluated with IBM SPSS Statistics for Windows, Version 20.0, IBM Corp, Chicago, IL.
Demography
Among 113 cases (Table 1), 64 cases (56.63%) were males and 49 cases (43.36%) were females. The maximum number of cases belongs to 41-50 years age group i.e 34 cases (30.08%) followed by 31-40 years age group i.e. 24 cases (21.23%).
| Age (years) | Males | Females | Total |
|---|---|---|---|
| 21-30 | 15 | 7 | 22 |
| 31-40 | 14 | 12 | 26 |
| 41-50 | 18 | 16 | 34 |
| 51-60 | 13 | 11 | 24 |
| 61-70 | 4 | 3 | 7 |
| Total | 64 (56.63%) | 49 (43.36%) | 113 |
Table 1: Patient’s demography.
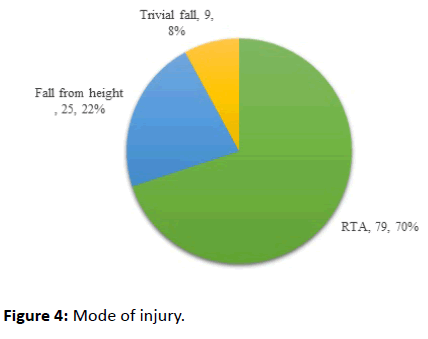
Mode of injury
Among 113 cases, 79 cases (69.91%) sustained an injury due to a road traffic accident, 25 cases (22.12%) fall from height and 9 cases (7.96%) due to trivial fall (osteoporosis) shown in Figure 4.
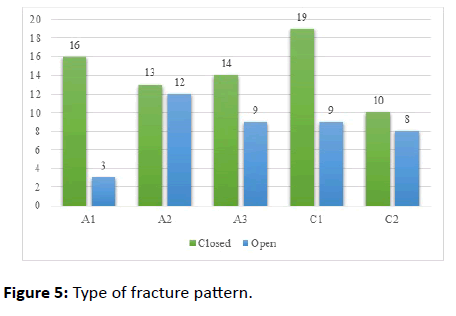
Type of fracture pattern
In our study, among 113 cases, according to AO classification, a total of 19 cases (16.81%) of A1 type, 25 cases (22.12%) of A2 type, 23 cases (20.35%) of A3 type, 28 cases (24.77%) of C1 type and 18 cases (15.92%) of C2 type of distal femoral fractures (Figure 5).
Classification of open fracture in terms with AO classification
According to Gustilo Anderson classification, type 1 compound cases were managed with tetanus toxoid and IV antibiotics pre-operatively. Type 2, 3a and 3b compound cases were managed with tetanus toxoid, IV antibiotic coverage and a thorough wound debridement (Table 2).
| AO classification | Grade of Gustilo Anderson system | |||
|---|---|---|---|---|
| Type 1 | Type 2 | Type 3a | Type 3b | |
| A1 | 2 | 1 | - | - |
| A2 | 4 | 4 | 3 | 1 |
| A3 | 1 | 2 | 4 | 2 |
| C1 | 2 | 3 | 3 | 1 |
| C3 | 2 | 3 | 2 | 1 |
Table 2: Classification of open fracture in terms with AO classification.
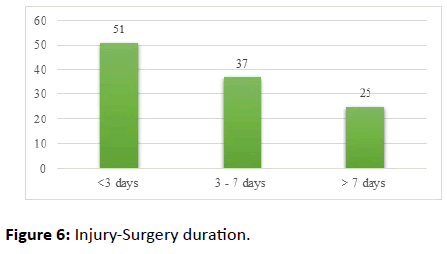
A total of 51 cases (45.13%) underwent surgery within 3 days of admission, 37 cases (32.74%) underwent between 3 to 7 days of admission after initial stabilization and 25 cases (22.12%) after 7 days of admission after aggressive treatment for control of infection (Figure 6).
Mode of reduction of fracture
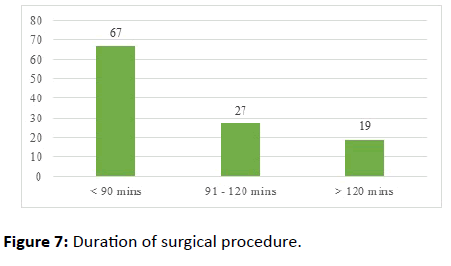
Among 113 cases, a total of 74 cases (65.48%) were reduced by closed reduction and 39 cases (34.51%) were reduced by open reduction of fractures. A total of 39 cases underwent an open reduction of fracture due to late presentation to the definitive management, inadequate reduction, improper immobilization and interposition of soft tissues. The cases which underwent open reduction were operated with increased operating time duration of more than 120 minutes (Figures 7 and 8).
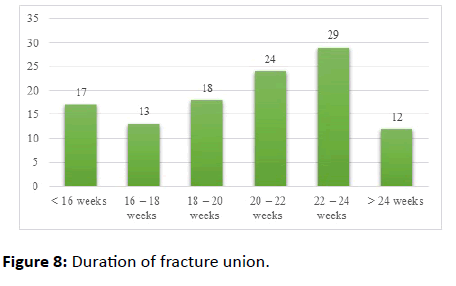
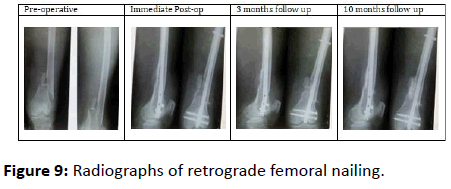
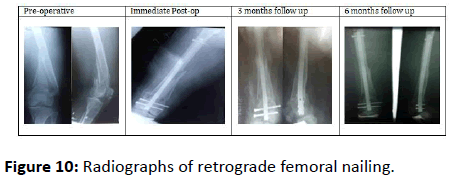
The mean duration of fracture union was 20.30 ± 2.13 weeks. All the cases were followed up serially as per our protocol with serial clinical and radiographical examinations (Figures 9 and 10).
Range of movements
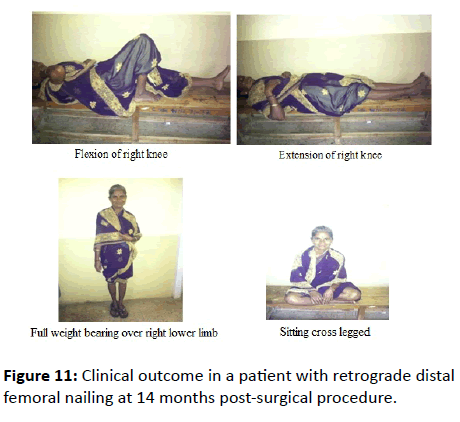
Out of 113 cases, at the end of 10 months follow up, 83 cases (73.45%) achieved ≥ 110°, 18 cases (15.92%) achieved 91°-109° and 12 cases (10.61%) achieved ≤ 90° of knee flexion. 12 cases with ≤ 90° of knee flexion were due to prolonged immobilization and delayed weight bearing of affected lower limb (Tables 3 and 4). The cases with a reduced range of knee flexion were treated with physiotherapy in the form of active and passive quadriceps strengthening exercises (Figure 11).
| Range of active flexion | ≤ 90° | 91°-109° | ≥ 110° |
| No of patients | 12 | 18 | 83 |
Table 3: Range of movements.
| Duration | Mean flexion at knee |
|---|---|
| At the end of 1st month | 41.20° ± 5.36° |
| At the end of 3rd month | 89.72° ± 11.41° |
| At the end of 6th month | 111.47° ± 9.01° |
| At the end of 12th month | 120.20° ± 15.27° |
Table 4: Mean flexion at the knee joint.
Complications
The most common complication encountered in our study was anterior knee pain 37 cases (32.74%), superficial infection at the nail insertion site 13 cases (11.50%), delayed union 7 cases (6.19%), non-union 3 cases (2.65%), limb shortening 3 cases (2.65%), varus angulation 6 cases (5.30%), valgus angulation 2 cases (1.76%) and breakage of nail in 2 case (1.76%).
The superficial infection at the nail insertion site was treated by IV antibiotics for 5 days followed by oral antibiotics for 5 days with regular dressings. The cases with anterior knee pain were managed conservatively with oral analgesics and offered nail removal after the satisfactory union of fractures. Delayed union cases were managed with dynamization. Non-union cases were managed with the opening of the fracture site, freshening of the fracture edges, opening of medullary cavity and internal fixation with either load sharing or load bearing device with adequate cancellous bone grafting. The cases with varus and valgus angulation got corrected in due course of bony remodeling after the nail removal. Nail breakage case went into non-union of fracture and later implant removal followed by locking compression plating was done.
Functional assessment by Lysholm knee scoring
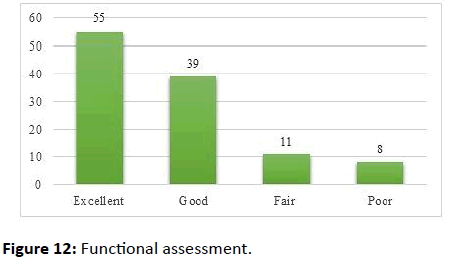
All cases were trained with active and passive joint mobilization exercises after the clinical sign of fraction union. The functional assessments were made with Lysholm knee scores (components-Limp, support, pain, instability, locking, swelling, stair climbing, and squatting). These scores were further graded as excellent (>90), good (84-90), fair (65-83) and poor (<65). Out of 113 cases, the functional outcome was excellent in 55 cases (48.67%), good in 39 cases (34.51%), fair in 11 cases (9.73%) and poor in 8 cases (7.07%). The poor range of movements (n=8) was due to non-union 3 cases, nail breakage 2 cases, limb shortening 3 cases (Figure 12).
The correlation analysis with Pearson’s correlation coefficient (r) was 0.8 which show a highly positive correlation between distal femoral fracture and retrograde distal femoral nailing.
Surgical implant removal
Clinically and radiologically united fracture patients were offered with implant removals which were done under locoregional anesthesia in an average of 30.32 ± 3.49 months.
Discussion
Out of all femoral fractures, the distal femoral fractures comprise approximately 3%-6% [1]. The mechanism of injury associated with distal femoral fractures may be of high-energy mechanisms such as motor vehicle accidents which are more common in the younger adults as compared with low-energy mechanisms such as fall from a stand in the elderly and osteoporotic patients [2]. Distal femoral fractures are associated with more complex soft tissue injuries, intraarticular and comminuted irrespective of etiology and thus challenge every orthopedic surgeon to achieve and maintain an adequate reduction and overall limb alignment [6].
The AO/OTA system is most universally used for distal femoral fracture classification. Fracture patterns include extraarticular (type A), partial articular/unicondylar (type B) and complete articular/bicondylar (type C). Further classification into subtypes of fractures indicates the progressively increasing degree of comminution [8]. The surgical management of distal femoral fractures is to promote early knee motion while restoring the articular surface, maintaining limb length and alignment, and preserving the soft-tissue envelope with a durable fixation that allows functional recovery during bone healing [9].
Intramedullary nails act as a load sharing device and provide the favourable intramedullary stability so that nails can be successfully implanted in bilateral or multisegmental fractures of the lower extremity. In addition, a variety of distal femur fractures ranging from AO type A and type C fractures can be stabilized. In our study, the retrograde intramedullary nailing method was being used and closed indirect fracture reduction was achieved by inserting the nail at a correct insertion point leaving the soft-tissue envelope intact.
Intra-articular AO type C fractures can be treated with the retrograde intramedullary nail, only if direct visualization and perfect reduction of the articular surface is possible. The distal interlocking screws of the retrograde nail have to be inserted at a valgus angle of approximately 7° to the joint line. So that the reconstruction of the physiological valgus angle of the femoral condyle and the femoral shaft is possible [10,11].
Dileep et al. in a case study of 21 cases concluded that retrograde IM nailing of distal femoral fractures was the reliable implant of choice for fracture stabilization with higher rates of union with minimal complications and without the interference of knee movements [12]. Hierholzer et al analyzed 115 patients with distal femur fracture who had been treated by retrograde IM nailing (n=59) or LISS plating (n=56). The functional results were analyzed with KOOS score and concluded locked plating can be used for all distal femur fractures including complex type C fractures, periprosthetic fractures, and osteoporotic fractures whereas intramedullary nailing provides favorable stability in bilateral or multisegmental fractures of the lower extremity and extra-articular fractures [13].
Shrihari et al. studied the biological and biomechanical advantages in distal femoral retrograde nailing in 30 patients. They reported excellent to good functional results in 73% of patients according to Lysholm knee scoring. The average knee range of movement was 106° and the average time to union was 16 weeks. They concluded that retrograde femoral nailing is an effective method for treatment of distal femoral fractures with advantages of reduced operative time, reduced blood loss and low incidence of complications [14]. Gupta SKV et al. [15] reported the limiting factors for retrograde distal femoral nailing were persistent anterior knee pain and inability to use in type C fractures whereas LCP plating was associated with less morbidity in type A distal femoral fractures. Locked plating may be utilized for all distal femur fractures including complex type C fractures and osteoporotic fractures [15].
The advantages of the retrograde femoral nail were uninterruption of fracture hematoma, decreased blood loss, soft-tissue protection due to a small incision, percutaneous joint fixation, the increased stability by the intramedullary loadsharing device. The disadvantages of retrograde nailing technique were lack of alignment control, posterior angulation, perforation of joint cartilage and intraarticular distribution of reaming debris [16-18].
In our study, 113 cases underwent surgical management with distal femoral retrograde nailing. The results were analyzed according to Lysholm’s knee scoring showed excellent in 55 cases (48.67%), good in 39 cases (34.51%), fair in 11 cases (9.73%) and poor in 8 cases (7.07%). The poor range of movements (n=8) were due to non-union 3 cases, nail breakage 2 cases, limb shortening 3 cases. The correlation analysis with Pearson’s correlation coefficient (r) was 0.8 which show a highly positive correlation between distal femoral fracture and retrograde distal femoral nailing.
Conclusion
Retrograde distal femoral nailing for AO/ASIF type A and type C distal a femoral fracture is a proven and reliable method of fixation. With minimal disruption to soft tissue and good purchase of the distal bone fragment, this approach provides stable fracture fixation, allowing early joint mobilization and weight bearing. The rate of union is high, with a low incidence of complications. The simplicity of the procedure also facilitates fracture fixation in patients with multiple trauma, including those with multiple fractures. This safe, successful, effective, reliable and useful technique should find a place in the armamentarium of every orthopedic surgeon dealing with distal femoral fractures that initially requires attention to details of the technique to prevent complication.
References
- Court-Brown CM, Caesar B (2006) Epidemiology of adult fractures: A review. Injury 37: 691-697.
- Kolmert L, Wulff K (1982) Epidemiology and treatment of distal femoral fractures in adults. Acta Orthop Scand 53: 957-962.
- Wilson JN (1982) Watson Jone’s: Fractures and joint injuries. (6thedn), pp: 1003-1070.
- Lupescu O, Nagea M, Patru C, Vasilache C, Popescu GI, et al. (2015) Treatment options for distal femoral fractures. Maedica J Clin Med 10: 117-122.
- Hartin NL, Harris I, Kaushik H (2006) Retrograde nailing versus fixed angled blade plating for supra-condylar femoral fractures: A randomized controlled trial. ANZ J Surg 76: 290-294.
- Ehlinger M, Ducrot G, Adam P, Bonnomet F, Jacob M, et al. (2013) Distal femur fractures. Surgical techniques and a review of the literature. Ortho Traum Surg Res 99: 353-360.
- Salem KH, Maier D, Keppler P, Kinzl L, Gebhard F (2006) Limb malalignment and functional outcome after antegrade versus retrograde intramedullary nailing in distal femoral fractures. J Trauma 61: 375-381.
- Marsh JL, Slongo TF, Agel J (2007) Fracture and dislocation classification compendium-2007: Orthopaedic Trauma Association classification, Database and Outcomes Committee. J Orthop Trauma 21: S1-S133.
- Rodriguez EK, Boulton C, Weaver MJ (2014) Predictive factors of distal femoral fracture nonunion after lateral locked plating: A retrospective multicenter case-control study of 283 fractures. Injury 45: 554-559.
- Sears BR, Ostrum RF, Litsky AS (2004) A mechanical study of gap motion in cadaveric femurs using short and long supracondylar nails. J Orthop Trauma 18: 354-360.
- Moed BR, Watson JT (1995) Retrograde intramedullary nailing, without reaming, of fractures of the femoral shaft in multiply injured patients. J Bone Joint Surg Am 77: 1520-1527.
- Dileep KS, Mahesha K (2016) Retrograde intramedullary nailing for fractures of distal femur: A prospective study. Int J Res Orthop 2: 276-279.
- Hierholzer C, Ruden CV, Potzel T, Woltmann A, Buhren V, et al. (2011) Outcome analysis of retrograde nailing and less invasive stabilization system in the distal femoral fractures, retrospective analysis. Ind J Ortho 45: 243-250.
- Shrihari LK, Mannual S, Sapan DS (2016) A clinical study of distal femoral fractures treated by retrograde femoral nailing-biological and biomechanical advantages with review of literature. Int J Ortho Traumatol Surg Sci 2: 371-377.
- Gupta SKV, Govindappa CVS, Yalamanchili RK (2013) Outcome of retrograde intramedullary nailing and locking compression plating of distal femoral fractures in adults. OA Orthopaedics 1: 23.
- Thompson AB, Driver R, Kregor PJ, Obremskey WT (2008) Long-term functional outcomes after intra-articular distal femur fractures: ORIF versus retrograde intramedullary nailing. Orthopedics 31: 748-750.
- Neubauer T, Ritter E, Potschka T (2008) Retrograde nailing of femoral fractures. Acta Chir Orthop Traumatol Cech 75: 158-166.
- Neer CS, Gratham SA, Shelton ML (1967) Supracondylar fractures of adult femur. J Bone Joint Surg Am 49: 591-613.
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences