The Effect of a Clinical Pathway Strategy for Managing Care in Total Joint Replacement: The Impact on Perioperative Outcomes
Schwarzkopf R, Zamansani T, Houng M, Bridgeman T
DOI10.4172/2471-8416.100011
Schwarzkopf R1*, Zamansani T2, Houng M2 and Bridgeman T2
1Division of Adult Reconstruction, Department of Orthopaedic Surgery, NYU Langone Medical Center Hospital for Joint Diseases, NY, USA
2University of California Irvine Medical Center, Orange, CA, USA
- *Corresponding Author:
- Ran Schwarzkopf
Assistant Professor, Division of Adult Reconstruction
Department of Orthopaedic Surgery
NYU Langone Medical Center Hospital For Joint Diseases
301 East 17th Street, New York, USA
Tel: 212-598-6000
E-mail: schwarzk@gmail.com
Received date: February 06, 2016; Accepted date: March 14, 2016; Published date: March 17, 2016
Citation: Schwarzkopf R, et al. The Effect of a Clinical Pathway Strategy for Managing Care in Total Joint Replacement: The Impact on Perioperative Outcomes. J Clin Exp Orthop. 2016, 2:11 doi: 10.4172/2471-8416.100011
Copyright: © 2016, Schwarzkopf R, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Introduction: The development of clinical pathways, for a variety of surgical procedures, has made an impact on clinical practice. When combined with the electronic medical record, clinical pathways can bring uniformity in orders and protocols designed to reduce error, decrease variability, and promote patient outcomes and safety. Our hypothesis is that the use of a modern evidence based clinical pathway will produce improved clinical outcomes in total joint replacement patients.
Methods: All patients undergoing primary total hip or knee replacement were selected to be included in this study. All participants were prospectively enrolled. As part of our clinical follow up, patients were assessed during their preoperative clinic visit and were followed 90 days postoperatively. Patient reported outcome measures were utilized to assess patient satisfaction and objective clinical outcomes.
Results: This report includes 102 patients who were followed for their progress while on the pathway. Overall there was an improvement in most of the measured outcome mean scores. There was a significant mean difference between preoperative and postoperative outcome measure scores for the following surveys: Harris Hip Score, Hip Knee Expectations Survey, HOOS Hip Score KOOS Knee Survey, Knee Society Score, WOMAC, SF-12, and UCLA Activity Score.
Discussion: We concluded that clinical pathways are a reliable tool that monitors the inpatient experience and processes of care in orthopedic surgery. The pathways support the accountability for outcomes of care and have proven superior to retrospective review and traditional quality assurance techniques.
Keywords
Joint replacement; Clinical pathways; surgical procedures
Introduction
The development of clinical pathways, for a variety of surgical procedures, has made an impact on clinical practice since the early 90’s. In addition to standardizing clinical practice, clinical pathways may define levels of cost effectiveness; reduce process and outcome variation; and support evidenced-based standards of care [1]. When combined with the electronic medical record, clinical pathways can bring uniformity in orders and protocols designed to reduce error, decrease variability, and promote patient outcomes and safety. Clinical pathways are associated with a reduction in-hospital complications and improved documentation without negatively impacting patients’ length of stay and hospital costs [2].
The Nationwide Inpatient Sample (NIS) shows that primary hip replacements increased by 48% from 153,080 procedures in 1997 to 225,900 in 2004. First-time knee replacements grew by 63% from 264,331 in 1997 to 431,485 in 2004. In 2009, more than 620,000 total knee arthroplasties (TKAs) were performed, and this number continues to increase annually. The demand for primary TKA is expected to grow by 673% to 3.48 million procedures by 2030 [3]. Annually, more than 300,000 THA procedures are performed in the US with a projected 137% increase by the year 2030 [3]. The implementation of clinical pathways for total joint replacement at our institution began in 2000 and continues today as a powerful strategy to manage care in this growing patient population. A previous study from our institution examined the use of clinical pathways as the driver of inpatient care in association with pre and post hospitalization outcome measurement tools related to physical and quality of life beyond hospitalization [4]. Due to ever changing technologies, clinical skills, and new orthopedic surgery faculty, we initiated the establishment of a Joint Replacement Surgical Home project, as part of a perioperative surgical home initiative. We hypothesized that clinical pathways have to be ever evolving with the advancement of clinical knowledge and surgical technique. We intend to demonstrate an improvement in overall patient outcomes and clinical management as a result of a more comprehensive updated clinical surgical home pathway. Our hypothesis is that the use of a modern evidence based clinical pathway will produce improved clinical outcomes in total joint replacement patients. The pathway is utilized as a tool to drive clinical practice. Pathways support the increased quality of the clinical outcomes by a continual review of the efficacy of standardizing care and evidence based best practices.
Methods
The study was part of a quality improvement initiative that followed the outcomes of our surgical home pathway. A review of the entire pre, intra, and post-hospitalization plan of care was conducted by an interdisciplinary team comprised of: a joint replacement fellowship trained orthopedic surgeon; Anaesthesiology; Pharmacy; Information Systems; Nursing; Physical Therapy; and, Decision Support. The evidence obtained in the development of evidence based clinical pathways was obtained from the University Health Consortium (UHC) and the Office Agency for Healthcare Policy Research and Quality (AHRQ).
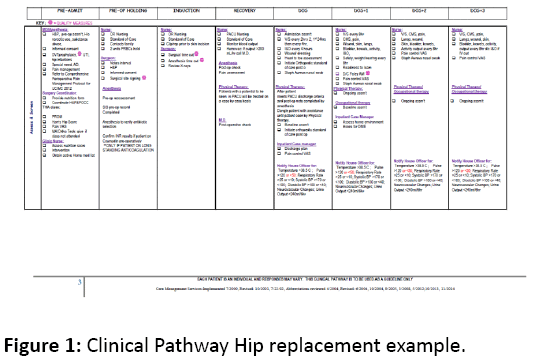
In addition, we used evidence-based best practice protocols from different professional association statements (such as the American Association of Hip and Knee Surgeons, American Academy of Orthopaedic Surgeons) and peer reviewed scientific publications as part of the Joint replacement perioperative surgical home. Each single element in our protocol is based either on evidence obtained from published clinical guidelines literature, or if such evidence does not exist, the protocol element was decided upon by the surgical home clinical leadership with a consensus agreement. The pathways were developed to meet the current standards of care and metrics used by the Center for Medicare Services (CMS) and other regulatory bodies. The perioperative teams were divided to examine perioperative, intraoperative and post-operative care. The Lean Six Sigma methodology was incorporated into the pathway affording the benefit of process mapping and identifying current state issues and potential future state solutions. Weak points were identified in process mapping and profiled in the clinical pathway (Figure 1). The GMLOS (Geometric Length of Stay) served as a benchmark in addition to the cost per discharge based on allocation of resources across the pathway. Length of stay for the hip and knee replacement in patients was 3 days and cost per discharge for hips and knees, known as the absolute cost, was determined by historical financial performance and comparison against the UHC (University Health Consortium) total cost per discharge data. In addition, financial historical data was retrieved from our institution’s Decision Support Department (financial and clinical utilization software system) and incorporated into the financial benchmark. Intra-operative performance was accomplished by line-by-line utilization in the OR in the presence of the Clinical Surgical Nurse IV specializing in joint replacement surgery.
The compliance to SCIP (Surgical Care Improvement Project) including: appropriate antibiotic selection; antibiotic duration of 24 hours: removal of foley catheter within 48 hours, and VTE prophylaxis were measures that were inserted into the clinical pathways. The clinical content of the pathways was then transferred to the associated electronic medical record (EMR).
Total joint replacement pathways include a comprehensive regimen for pre-and post- operative anti-coagulation treatment. The pathways addressed the following: perioperative management of patients on Warfarin; patients at high risk for cardiac events (exclusive of coronary stents); patients at low risk of cardiac events; and perioperative management of patients on chronic opioids. The pathways were then built into the sophisticated EMR (Allscripts, Chicago, ILL. Sunrise Acute Care, Atlanta, GA 2008). Data acquisition was achieved through the interface between the hospital’s Decision Support System and the Allscripts system. Once the order set is accessed a patient is registered against the appropriate clinical pathway. Compliance to the pathway metrics are then displayed in preparation for reporting to the authoring physician, the Orthopedic Administrative Committee and Executive Leadership for the Medical Center.
The measurement of the total joint replacement clinical Pathways began 4 months after implementation and focused on: volume; cost per discharge; length of stay; VTE prophylaxis compliance; and VTE as a secondary diagnosis in the acute environment. Physician performance in relationship to length of stay and cost per discharge was reflected in a scatter gram with aggregated data obtained from the Decision Support System.
Additionally, the EMR order set utilization was reviewed to determine percent of utilization, which is synonymous with the use of the appropriate clinical pathway.
Sample selection and data collection
All patients undergoing primary total hip or knee replacement were selected to be included in this study. All participants were prospectively enrolled between 10/2012-10/2014. As part of our clinical follow up, patients were assessed during their preoperative clinic visit and were followed 90 days postoperatively.
The patient demographics and pre-operative factors that were evaluated for each patient included: gender, age, BMI, living status, employment status, diet, pre-operative exercise, alternative medicine use prior to surgery, and smoking history. Patient reported outcome measures were utilized to assess patient satisfaction and objective clinical outcomes: WOMAC [5] Knee Society Score System [6,7], Harris Hip Score [8], Hip Knee Expectations Survey, Knee injury and Osteoarthritis Outcome Score (KOOS) [8,9], Hip disability and Osteoarthritis Outcome Score (HOOS) [10], UCLA activity score [11,12], SF-12 physical (PCS) and mental component scores (MCS) [13,14] Timed Get Up and Go score (TGUG) [15], and EuroQol-5 dimension (EQ-5D) score [16].
Patients who had any other type of total joint replacement surgeries were excluded from these analyses.
Data analysis
Descriptive data are expressed as percentages and means with standard deviations. Changes in survey results were calculated by the difference in the mean scores between baseline and follow up period. Means and proportions were calculated for the entire sample and separately for total hip and knee replacement. Total hip and knee replacement patients were compared in terms of their preoperative characteristics using chi-square and t-tests when appropriate. No statistically significant differences were found based on preoperative characteristics between the groups, therefore groups were combined for subsequent analyses to consolidate findings and increase the power of the analyses. Pre and post survey score were compared and the mean differences, standard deviation (SD) and 95% confidence intervals (CI) are reported. We used SPSS (SPSS Inc., Chicago, IL v.9.3) for all analyses.
Results
This report includes 102 patients who were followed for their progress while on the pathway. Of the 102 patients 63.7% were female and 36.3% male. Overall patients’ mean age was 67 years (SD± 11.4 years) with 51 % Caucasian and predominantly nonsmokers (90.2%). Patients mean body mass index (BMI) was 29.8 (SD ± 6.5 kg/m2). Nearly sixty four percent were inactive (63.7%) and more than half of the patients were married (Table 1).
| Entire sample | Knee | Hip | p | |
|---|---|---|---|---|
| (n = 102) | (n =71) | (n=31) | ||
| Age in years, mean ± SD* | 67 ± 11.4 | 68 ± 9.4 | 65± 14.8 | 0.2 |
| Female, n (%) | 65 (63.7) | 50 (70.4) | 15 (48.4) | |
| Caucasian, n (%) | 52 (51.0) | 36 (50.7) | 16 (51.6) | |
| Body mass index, mean kg/m2 ± SD* | 29.8 ± 6.5 | 30.7 ± 5.9 | 27.8 ± 7.4 | 0.06 |
| Smoking, n (%) | 11 (10.8) | 8 (11.3) | 3 (9.7) | |
| Exercise, N (%) | 37 (36.3) | 25 (35.2) | 12 (38.7) | |
| Retired, N (%) | 77 (75.5) | 58 (81.7) | 19 (61.3) | |
| Not Married, n (%) | 46 (47.0) | 33 (46.5) | 15 (48.4) | |
| Living alone, n (%) | 20 (19.6) | 12 (16.9) | 8 (25.8) | |
| Medicare Insurance, N (%) | 42 (40.2) | 30 (42.3) | 12 (38.7) |
Table 1: Sample subject characteristics.
There were 71 total knee replacement surgeries and 31 total hip replacement surgeries. Patients undergoing total knee replacement were mostly older (mean age 68 years) female (70.4%), with higher BMI compared to the patients undergoing total hip replacement (30.7 kg/m2) (Table 1).
The preoperative to postoperative scores did not demonstrate gender- specific differences and additional gender specific analyses did not show any differences between knee and hip replacement. The average age of the female patients was similar (p=0.10). Females had a higher percentage (70.4%) of primary total knee replacement surgery.
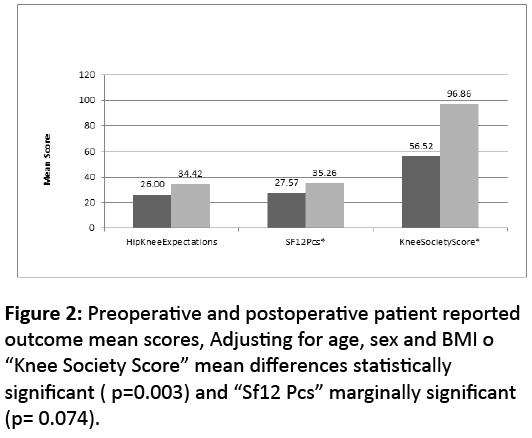
Overall there was an improvement in most of the measured outcome mean scores. There was a significant mean difference between preoperative and postoperative outcome measure scores for the following surveys: Harris Hip Score, Hip Knee Expectations Survey, HOOS Hip Score KOOS Knee Survey, Knee Society Score, WOMAC, SF-12, and UCLA Activity Score (Table 2). Statistically significant mean difference with univariate analyses was also observed for Hip Knee Expectations Survey, Knee Society Score, and SF-12 (Table 2). After adjusting for age, gender and BMI “Knee Society Score” mean differences remained statistically significant (p=0.003) and SF-12 marginally significant (p= 0.074) (Figure 2).
| Preoperative Mean ± SD | Postoperative Mean ± SD | P Value | |
|---|---|---|---|
| N =102 | |||
| PreopEq5DL | 64.67 ± 19.78 | 64.91 ± 21.12 | .962 |
| Get up and Go Scores | 15.98 ± 8.98 | 14.01 ± 6.84 | .519 |
| Harris Hip Score* | 34.00 ± 21.39 | 71.29 ± 19.24 | 0.001 |
| Hip Knee Expectations Survey* | 26.00 ± 10.12 | 34.423 ± 13.24 | 0.003 |
| Hoos Hip Score* | 23.10 ± 25.16 | 80.60 ± 11.71 | 0.005 |
| Knee Society core* | 56.52 ± 21.69 | 96.86 ± 35.95 | <0.0001 |
| Womac* | 29.63 ± 18.04 | 76.99 ± 15.35 | <0.0001 |
| Sf12 Mcs* | 46.20 ± 11.34 | 50.82 ± 10.96 | .099 |
| Sf12 Pcs* | 27.57 ± 5.68 | 35.26 ± 9.59 | .001 |
| Koos Knee Survey* | 34.32 ± 9.97 | 69.68 ± 22.65 | <0.0001 |
| UCLA Activity Score* | 2.54 ± 1.13 | 4.62 ± 1.71 | .007 |
Table 2: Preoperative and postoperative Mean value, standard deviation, and test significance.
GMLOS benchmark was 3.0 and the actual ALOS exceeded expectations with an average of 2.0 for Knee and 2.8 for Hip. There were no incidences of DVT as a secondary diagnosis, during the acute hospitalization phase. Percent of order set use/clinical pathway was at 100%.
There was 100% of VTE prophylaxis use (Heparin, Warfarin, or Low molecular weight heparin). The use of sequential compression devices (SCD) was at 100%. Compliance to SCIP metrics regarding antibiotic selection and duration, and Foley removal within 48 hours was 100%.
Discussion
This current study demonstrates that the utilization of the enhanced clinical pathways, under the PSH initiative in managing care, is an effective method to monitor the process of acute clinical care in patients undergoing primary total joint replacement surgery.
It is important to note that it took 6 months before implementation of the clinical pathways in which a number of refinements regarding appropriate antibiotic use were required. In-depth discussions with Physical Therapy, regarding early ambulation of the patient, and training for nursing to initiate ambulation after 4pm on the day of surgery was a significant achievement during implementation of the pathway. Additional discussions were held regarding the use of tranexamic acid and the impact on transfusion rates and cost per discharge as well as antibiotic selection for the penicillin allergic patient with the Antibiotic Stewardship Committee. We experienced one computer interface system issue regarding the clinical path order set acquisition, which resulted in flawed data reflecting marginal use of the pathways, this was corrected and pathway use was marked as 100%. Finally, the initial use of tranexamic acid was not properly included by Decision Support, which reflected an increased cost per discharge over the clinical path cost estimation, which was incongruent to a shorter ALOS. This led to reevaluation of cost capture and correction of inaccuracies.
Patient-derived outcome scales have become increasingly more critical to physicians and clinical researchers for measuring improvement in function after surgery. Responsive outcome instruments for total hip and knee replacement are important for scoring system’s ability to detect clinically important changes over time [17]. The goal of our study was also to evaluate the ability of health-status instruments to measure early functional recovery after total hip and total knee arthroplasty.
Pre and post-operative measurement of activity and the quality of life demonstrated improvement in both hip and knee replacement surgeries. However results differ, depending on the evaluation assessment tool. The Knee Society Score may be a more a sensitive tool for the assessment of outcome after TKA. Thus, increasing age or a medical condition will not affect the measured knee score [18].
Limitations
This study presents some limitations that should be considered. The sample size is not representative of the whole population. Lately there is a move towards simple or even single-question instruments for assessing patient outcome [19]. While the use of multiple functional outcome questionnaires is a valuable practice, we would recommend limiting the number of questionnaires which would promote an increase survey response rate and a decrease in data administration and collection efforts. In addition we would anticipate a reduction in the number of questionnaire would increase the pre-operative patient experience as well as increasing response rate and improving power of the study [20].
Another limitation of the present study is the limited follow up time. After 3 months, it was not clear whether a post improved score following joint replacement was truly indicative of full functional recovery. Many patients are generally believed to have continued improvement beyond three months, which we did not measure after 3 months and beyond. However the results are indicative of even a higher patient outcome improvement beyond the 3 months. This is also consistent with findings that greater improvement is generally realized for patients managed with longer (6 to 12 months) postoperative interval follow up [21].
Larger multicenter initiatives are needed to evaluate the proper impact standardized protocols have on hospital systems. We presented 100% pathway usage but this can be biased by the fact that only one institution was examined with a very rigid compliance.
Conclusion
We concluded that clinical pathways are a reliable tool that monitors the inpatient experience and processes of care in orthopedic surgery. The pathways support the accountability for outcomes of care and have proven superior to retrospective review and traditional quality assurance techniques. Joint replacement clinical pathways have promoted collaborative practice between all disciplines. To date, high volume and clinically applicable diagnoses continue to be identified with the Peri-Operative Surgical Home project at our Medical Center.
The value of managing care through carefully constructed clinical pathways has proven to be a model for clinical quality improvement. New concepts of continual quality improvement incorporating regulatory metrics have been rapidly introduced to gain competitive advantages in the market place and as indicators for clinical excellence.
The expectation is that high volume high cost procedures will be selected to fall under the surgical home project. These efforts will be focused on promoting the standardization of health with quality clinical outcomes for the patients we serve.
References
- Rotter T, et al. (2010) Clinical Pathways: effects on professional practice, patient outcomes, length of stay and hospital costs. Cochrane Review 3: CD006632.
- Dean A Seehusen (2010) LTC, MC, USA, MPH. Evans Army Community Hospital, Fort Carson Colorado. Am Fam Physician 82: 1338-1339. Elders MJ (2008) Hip and Knee implant review. Orthopaedic network news 19: 1–20.
- Tania Bridgeman, Harry Skinner, Tahereh Zamansani, Michele Schulz (2010) Hip and knee replacement continuum of care: combining clinical and functional outcome measurement. International Journal of Care Pathways 14: 102-108.
- American College of Rheumatology (2013) Western Ontario and McMaster University Osteoarthritis Index (WOMAC).
- John N Insall, Lawrence D Dorr, Richard D Scott, Norman Scott W (1989) Rationale of The Knee Society Clinical Rating System 248: 13-14.
- Noble PC, Scuderi GR, Brekke AC, Sikorskii A, Benjamin JB, et al. (2012) Development of a new Knee Society scoring system. ClinOrthopRelat Res 470: 20–32.
- Anna Nilsdotter, Ann Bremander (2011) Measures of Hip Function and Symptoms Harris Hip Score (HHS), Hip Disability and Osteoarthritis Outcome Score (HOOS), Oxford Hip Score (OHS), Lequesne Index of Severity for Osteoarthritis of the Hip (LISOH), and American Academy of Orthopedic Surgeons (AAOS) Hip and Knee Questionnaire. Arthritis Care & Research 63: S200–S207.
- Roos EM, Roos HP, Lohmander LS (1998) Knee injury and osteoarthritis outcome score (KOOS)—development of a self-administered outcome measure. J Orthop Sports PhysTher 28:88–96.
- Knee injury and Osteoarthritis Outcome Score.
- Nilsdotter AK, Lohmander LS, Klassbo M, Roos EM (2003) Hip Disability and Osteoarthritis Outcome Score (HOOS)- Validity and responsiveness in total hip replacement. BMC Musculoskeletal Disorders 4: 10-11.
- Naal FD, Impellizzeri FM, Leunig M (2009) Which is the best activity rating scale for patients undergoing total joint arthroplasty? ClinOrthopRelat Res 467: 958-965.
- Christina C Wee, Roger B Davis, Mary Beth Hamel (2008) Comparing the SF-12 and SF-36 health status questionnaires in patients with and without obesity.Health and Quality of Life Outcomes 6:1.
- SF-12® Health Survey Scoring Demonstration.
- Rehab Measures: Timed Up and Go.
- EQ-5D-5L. User Guide: Basic information on how to use the EQ-5D-5L instrument.
- Robert G Marx, Edward C Jones, Nawal C Atwan, Robert F Closkey, Eduardo A Salvati, et al. (2005) Measuring Improvement Following Total Hip and Knee Arthroplasty Using Patient-Based Measures of Outcome. J Bone Joint Surg Am 87: 1999 -2005.
- John N Insall, Lawrence D Dorr, Richard D Scott, W Norman Scott (1989) Rationale of The Knee Society Clinical Rating System; Clin Orthop 248: 13-14.
- Arden NK, Kiran A, Judge A (2011) What is a good patient reported outcome after total hip replacement? Osteoarthritis Cartilage 19: 155–162.
- Guyatt G, Walter S, Norman G (1987) Measuring change over time: assessing the usefulness of evaluative instruments. J Chronic Dis 40: 171-8.
- Bachmeier CJ, March LM, Cross MJ, Lapsley HM, Tribe KL, et al. (2001) Arthritis Cost and Outcome Project Group. A comparison of outcomes in osteoarthritis patients undergoing total hip and knee replacement surgery. Osteoarthritis Cartilage 9: 137-46.
- Anderson JG, Wixson RL, Tsai D, Stulberg SD, Chang RW (1996) Functional outcome and patient satisfaction in total knee patients over the age of 75. J Arthroplasty 11: 831-840.
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences