Working with Orthopedic Oncologists: When to Offer Immediate and when and why to Delay Definitive Reconstruction of an Extremity
Marek Dobke, Gina A Mackert, Amanda Goldin and Anna Kulidjian
DOI10.4172/2471-8416.100037
Marek Dobke1*, Gina A Mackert2, Amanda Goldin3 and Anna Kulidjian3
1Division of Plastic Surgery, Department of Surgery, University of California San Diego, San Diego, CA, USA
2Department of Hand, Plastic and Reconstructive Surgery, Burn Care Center, Department of Plastic Surgery of the University of Heidelberg, BG Trauma Center Ludwigshafen, Ludwigshafen, Germany
3Department of Orthopedics, University of California San Diego, San Diego, CA, USA
- *Corresponding Author:
- Marek K Dobke
Division of Plastic Surgery
University of California San Diego
San Diego, CA, USA
Tel: 619 543 6084
E-mail: mdobke@ucsd.edu
Received date: August 08, 2017; Accepted date: September 05, 2017; Published date: September 08, 2017
Citation: Marek KD, Gina AM, Amanda G, Anna K (2017) Working with Orthopedic Oncologists: When to Offer Immediate and when and why to Delay Definitive Reconstruction of an Extremity. J Clin Exp Orthop Vol.3:37. doi: 10.4172/2471-8416.100037
Copyright: © 2017 Marek KD, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
A review of patients that were treated jointly by the plastic and the orthopedic surgery teams from 2011 to 2015 to evaluate the timing of definitive reconstruction of extremity defects was undertaken. The cohort consists of 81 patients, of which 4 presented with either a high-risk lesion or an advanced squamous cell carcinoma and of which the remaining 77 patients presented with different types of extremity sarcomas. In 58 cases, immediate-definitive reconstruction was performed, while in 23 cases the definitive procedure was delayed. Immediate definitive reconstruction, concurrent with ablative procedures, was offered whenever possible. In 16 cases, delayed reconstruction was due to diagnostic uncertainty (uncertain diagnosis per se or non-established negative margins). In 6 cases, delayed reconstruction was performed because of infection, in 1 case a bleeding disorder necessitated workup and in another, the intraoperative histology necessitated a plan-change, wound temporization and preparation of an arteriovenous fistula for microsurgical reconstruction. Indications for delayed reconstruction can be related to systemic conditions, donor or recipient site issues (infection, suspicion of margin-problems or tumor “not in continuity”). Although frozen sections have an overall diagnostic accuracy of 90%, changes in management were related to the inadequacy of frozen material, sampling errors resulting from heterogeneity or non-appositional growth of malignancy. A high rate (28%) of delayed reconstruction corresponds with new data reaffirming an old paradigm (radically excised margins “make a difference”), and with objectives dictated by customized, personalized, multimodal approaches. Wound temporization was offered whenever definitive reconstruction couldn’t be performed immediately. Limb sparing, with the utilization of temporary spacers or distractors, mega-prostheses, or trials of re-implanting formerly tumorous bone autografts, which have been sterilized to eliminate malignant cells – may all necessitate temporary coverage or staged repair. Authors’ clinical experience was evaluated in the context whether the rationale behind immediate versus delayed reconstruction was optimal.
Keywords
Oncological extremity defect; Immediate reconstruction; Delayed reconstruction
Introduction
It is commonly believed that patients undergoing immediate functional reconstruction for extremity sarcoma resection may achieve what is judged to be a very a good to excellent result with immediate, definitive reconstruction [1,2]. The addition of immediate microsurgical free tissue transfer for reconstructive purposes greatly extends the limits of limb salvage [1,3]. Although the results of immediate major reconstruction can be very impressive, there are also cautionary reports regarding the performance of immediate reconstruction when there are uncertainties, errors and problems with the diagnosis. Cases where the diagnosis was not firmly established or confirmed, or where the focus was set on sparing the extremity instead of focusing on a long-term cure or patient survival under an established diagnosis, make an argument for delaying definitive reconstruction. Although not always possible in a preoperative or intraoperative setting, collecting the patient’s complete clinical information may require the delay of reconstruction, but the delay may reduce the need for additional surgeries resulting from an inaccurate diagnosis or an uncertain situation regarding the margins [4-9]. Statistics such as a 25% chance of recurrence after a wide excision of an extremity soft tissue sarcoma, and up to a 95% chance of a high-risk cutaneous squamous cell carcinoma development (e.g., patients with bullous disease, immunosuppressed organ transplant recipients, scar-originating malignancy, deep or perineural invasion) within five years after primary excision, reaffirm the value of staged or delayed definitive reconstruction. Delayed reconstruction enables completion of the margin-analysis and planning of the multimodal management of the extremity sarcoma [5,9,10].
For the multidisciplinary plastic and orthopedic surgical teams, the prospect of the best functional outcome is not only related to the concept of anatomical extremity salvage, but also to the ability of performing complex anatomical and functional reconstructions. In other words, if performed without certainty of the diagnosis or the presence of clear margins, or in the event of a change in the clinical situation, the possibility that such a reconstruction might have to be revised or discarded in the future presents an argument for delayed reconstruction or at least a customized approach with defect temporization until all necessary information is known [7,11-13].
On the contrary, there are clinical scenarios that necessitate definitive immediate soft tissue reconstruction. Post-ablative or post-amputative defects may be so massive that some form of immediate reconstruction is mandatory. Sometimes post-amputative extremity parts may be utilized as a donor site for a flap. In such instances, there is no other technical maneuver or choice other than to proceed with immediate reconstruction [14,15]. For recurrent disease with margins that have not yet been completely analyzed, scenarios with known frequent disease recurrences or in cases of planned alternative therapy options (e.g., adjuvant radiation therapy), muscle flaps loaded with brachytherapy catheters as a choice for reconstruction may be used [13,16].
Long term prognostic models have not yet been developed and it is unknown how the combination and the sequencing of the treatment modalities impacts the chance for a permanent cure [4,7,10,17]. The goal of this study was to critically analyze the authors’ clinical experience and evaluate whether the rationale regarding the choice of immediate versus delayed reconstruction was optimally balanced. In addition, a preliminary itemization of factors, known prior to ablative surgery, characterizing patients who underwent delayed definitive reconstruction was made, in an attempt to determine if these factors could be applied for the development of a propensity score for the selection of the reconstructive treatment method to ensure the best possible outcome (e.g., no re-resections, no local recurrence, good functional outcome, no amputative surgery, and good survival) [18].
Materials and Methods
The author’s combined database includes 81 patients with advanced or complex post-malignancy extremity reconstruction. All cases necessitated multidisciplinary planning and surgical interventions (resection by orthopedic oncology and reconstruction by plastic surgery). The 81 patients (45 males and 36 females) were treated between January 2011 and December 2015 with an average age of 45 years (range 12 to 80 years). The tumor types within the study population are presented (Table 1).
| Tumor type | Number of patients (%) |
|---|---|
| Advanced squamous cell carcinoma | 4 (5%) |
| Clear cell carcinoma | 2 (2%) |
| Liposarcoma | 6 (7%) |
| Malignant fibrous histiocytoma | 7 (9%) |
| Epitheloid sarcoma | 6 (7%) |
| Osteosarcoma | 15 (19%) |
| Synovial cell sarcoma | 10 (12%) |
| Fibrosarcoma | 8 (10%) |
| Chondrosarcoma | 6 (7%) |
| Recurrent dermatofibroma protuberans with fibrosarcoma | 2 (2%) |
| Leiomyosarcoma | 7 (9%) |
| Ewing sarcoma | 6 (7%) |
| Rhabdomyosarcoma | 2 (2%) |
Table 1: Histopathological diagnoses in the study population.
Anonymized records of the multidisciplinary treatmentplanning conferences were reviewed for individual patient age at diagnosis, sex, tumor site, type and duration of signs and symptoms, type of previous treatment (if any), initial diagnosis, local recurrences, regional or distant metastatic involvement, and the outcome as of December 2015. For each individual case, treatment-planning was reenacted and factors determining the choice of the timing of the post-resection reconstructive strategy were tabulated. Utilizing the concept of “decision-analysis” on a continuum regarding diagnostic certainty and the probability of a certain diagnosis (no diagnosis versus diagnosis/ information uncertain versus diagnosis established), the threshold for further testing accompanied by delayed reconstruction and preparational wound temporization versus definitive immediate reconstruction was determined. In an attempt to quantify factors helping in determining the clinical decision, factors (one point for each factor) were assessed retrospectively during treatment-planning conferences. These factors were termed Choice Determining Points (CDP). CDPs were determined by collation of commonly quoted predictors of the margin status (tumor histology, tumor size, patient age, etc.) [4,9,10,19-21]. It was hypothesized that CDPs determine the suitability of an indication calling for an immediate reconstructive approach. The CDPs were assigned to determine a potential threshold for a specific decision, attempting to develop a rational, quantitative approach for a formulation of clinical guidelines on when to use immediate versus delayed reconstruction for possible future application (Table 2) [17,19]. In the analyzed cases, no decisions were made based on the number of CDPs.
| Established diagnosis |
| Certainty about safe margins |
| Ability to perform major reconstruction concomitant to resection with low risk (anaesthesia, complications related to concurrent infection, bleeding disorder, etc.) |
| Ability to perform reconstruction as a single stage procedure |
| Completion of neoadjuvant treatment (if any) |
| Ability to complete definitive reconstruction without delaying adjuvant treatment (if indicated) |
| Ability to combine reconstruction with adjuvant therapy (e.g., brachytherapy) (if indicated) |
| Primary tumor size<5 cm |
| Patient age<50 years |
| Low tumor grade |
| No recurrent tumor |
| No evidence of presence of metastatic disease |
| *CDP=Choice Determining Points |
Table 2: Factors influencing the choice of definitive immediate extremity reconstruction (CDPs)
The selection of the reconstructive technique, the combination of reconstructive options, the type of wound temporization with or without utilization of wound sealing, negative pressure therapy or skin substitutes, was based on general plastic surgery principles. In 12 cases, more than one reconstructive option was utilized. Primary closure was utilized in 2 cases, skin grafts were used in 23 cases, local skin or fasciocutaneous flaps in 26 cases, pedicled myocutaneous in 35 cases, and free fasciocutaneous, muscle, myocutaneous or osteocutaneous flaps in 7 cases. One microsurgical free flap based repair was performed as immediate reconstruction and the remaining cases were conducted as delayed procedures.
Results
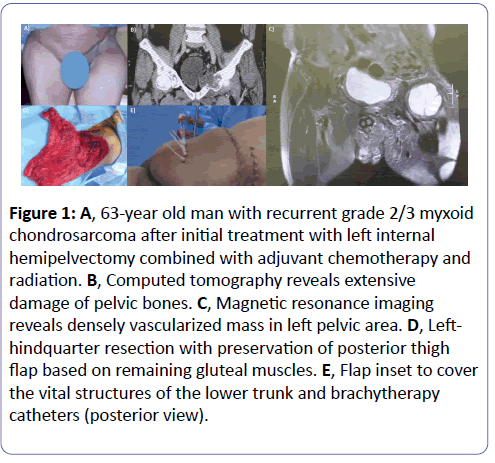
In 58 cases, resection was followed by immediate-definitive reconstruction, while in 23 cases the definitive procedure was delayed. Whenever feasible, during the original treatment planning, immediate definitive reconstruction, concurrent with ablative or amputative procedures, was offered. Retrospective analysis revealed that all patients but six, which were offered immediate reconstruction, were categorized as meeting all CDPs listed in Table 2. The six patients that did not meet all CDPs were aged 50 years and older, and two of these six were also treated for recurrent disease. The follow up (from one month to five years) revealed fatal progress of the disease in three cases (1. osteosarcoma of the humeral bone after a forequarter amputation, 2. pleomorphic malignant shoulder soft tissue fibrous histiocytoma and 3. pelvic chondrosarcoma) and local recurrence requiring left upper extremity amputation in one case of myxoid sarcoma of the elbow area, while the remaining patients appear to be disease free. Two of the latter patients underwent immediate reconstruction to cover not only critical defects but to accommodate flaps for the placement of brachytherapy catheters (Figure 1).
Figure 1: A, 63-year old man with recurrent grade 2/3 myxoid chondrosarcoma after initial treatment with left internal hemipelvectomy combined with adjuvant chemotherapy and radiation. B, Computed tomography reveals extensive damage of pelvic bones. C, Magnetic resonance imaging reveals densely vascularized mass in left pelvic area. D, Left-hindquarter resection with preservation of posterior thigh flap based on remaining gluteal muscles. E, Flap inset to cover the vital structures of the lower trunk and brachytherapy catheters (posterior view).
Of the 23 delayed reconstruction cases, 16 cases had delayed reconstruction offered because of diagnostic uncertainty (uncertain diagnosis per se or non - established clear or safe margins) during the original pre-surgery treatment-planning conference. In 6 cases, delayed reconstruction was performed due to an infection of the diseased site, which needed to be brought under control prior to reconstruction. In addition, one of these cases demonstrated a bleeding disorder and in 1 further case, the intraoperative histology necessitated a change of plans, wound temporization and preparation of an arterio-venous fistula for the subsequent microsurgical reconstruction. Retrospective analysis revealed that only one of these cases met 11 of the 12 CDPs and the remaining 22 patients had a maximum of 9 CDPs (average 7 CDPs) (Table 3).
| CDP | Number/% |
|---|---|
| Non-established diagnosis (which includes cases of changing diagnosis) | 2 (9%) |
| Lack of certainty regarding appropriate margins (Figure 4) | 16 (70%) |
| High local or general risk for major procedure, significant co-morbidities | 8 (35%) |
| Technical inability to perform reconstruction as a single stage procedure (Figure 5) | 2 (9%) |
| Non-completion of neoadjuvant treatment | 2 (9%) |
| Concern about delaying adjuvant treatment | 2 (9%) |
| Tumor size>5 cm (Figure 3) | 2 (9%) |
| Patient>50 years | 2 (9%) |
| Recurrent tumor and need to rule out satellite tumors, regional and distal metastatic lesions | 4 (17%) |
| Presence of evidence of distant metastatic disease | 3 (13%) |
Table 3: Factors characterizing patients who underwent the delayed definitive reconstruction as they were known prior to ablative surgery. All but one of the 23 patients in these groups were characterized by more than one CDP (Choice Determining Point).
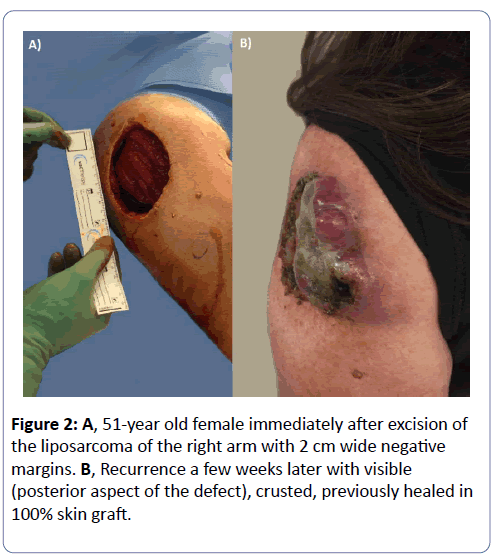
This specific patient with 11 CDPs, who’s case demonstrated the importance of being cautious regarding the timing of reconstruction, received a temporary wound coverage with Integra (Integra LifeSciences, Plainsboro, NJ) after wide excision of a liposarcoma with clear margins while waiting for the results of the tumor grading (results revealed a moderate grade) (Figure 2).
Immediately after tumor excision, the wound was covered with Integra (Integra LifeSciences, Plainsboro, NJ) while histopathological assessment, including tumor grading, was finalized. Four days after the excision, the patient underwent placement of a split thickness skin graft without further re-excision. The graft initially healed, however, two weeks later (4 weeks after excision), the patient developed a local recurrence and succumbed to metastatic disease a few months later [6,22,23].
The tabulation of the number of CDPs of patients, who underwent delayed definitive reconstruction, is depicted in Table 3. Reassessment of the data/information available to treating physicians at the time of the original, pre-resection management-planning or intraoperative situation did not result in a single stipulation that the plan regarding the immediate versus delayed reconstruction should be different from the management plan, which was implemented.
Discussion
The definition of the best surgical treatment from the standpoint of function, preservation, curation, and quality of life is controversial. The lowest rate of recurrence is found in patients with amputative or compartmental (radical) resections [4,5,7,10,24,25]. However, wide, radical excisions or amputative surgery may result in a significant loss of tissue, especially if the tumor is large in diameter. On the other hand, conservative excisions with marginal margins may result in tumor rupture or local tissue contamination with tumor cells and are associated with higher rates of local recurrence [1,2,4,22,24,25]. Safe surgical margins are a condition sine qua non for optimal long term results. The definition “how much margin is safe” has evolved due to a better understanding of the biological mechanisms of malignancies and, as a result of the expansion of available management options for advanced extremity malignancies, in terms of surgical, including rehabilitative, and non-surgical therapeutic modalities, leading to an increased complexity of clinical decision making [1,2,4,7,10,11,17]. Nevertheless, the pivotal point for reconstructive considerations and CDPs that can be controlled by the patient and the surgeons, are surgical margins. Therefore, it is of no surprise that the majority of reconstructive dilemmas evolve from diagnosis and/or issues related to the margin(s) [4,7,25]. As the recognition and the increased knowledge about the heterogeneity of sarcomas leads to personalized management plans, CDPs may become a useful, evidence based tool for planning the reconstructive approaches. Highlighting these points may aid in surgical planning, promote an increased intraoperative awareness of high risk situations, reduce local recurrence, and perhaps increase the overall survival after surgery.
This study was not powered to detect whether immediate versus delayed reconstructive approaches impact the core oncological outcomes. The intent of the introduction of the CDP concept was to obtain preliminary insight into the potential usefulness of a reference determining if a “score” based system could be utilized to justify immediate or delayed reconstruction as an adjunct in the decision-making process. The question arises, whether immediate reconstruction is safe when the majority of CDPs are known or if the only acceptable threshold for recommending immediate reconstruction should be at the level of 100%, meaning all of the CPDs are met and/or known. At this time, this part of the study was rather designed to identify features of patient stratification to ensure optimal outcomes. The sample is not robust enough to provide statistical data on the CDPs. However, as the clinical experience and CDP data collection grows, it will perhaps be possible to determine the statistical significance associated with reaching a specific threshold of CDP. In the case of the liposarcoma mentioned earlier in this paper (Figure 2) (the patient met 11 of 12 CDPs), the excision was conducted generously with an at least 2 cm wide radial margin declared negative by pathology. The reconstruction was delayed for a few days for a relatively non-critical reason (determination of the grade of differentiation of the liposarcoma). The question arises whether the delay of reconstruction could also be utilized to pathologically reevaluate the margins, or to conduct additional tests, for example for the determination of circulating markers of “tumor-virulence”, presence of infiltrative patterns of spread of growth, probable dedifferentiation, such as miRNA-155, or perhaps for re-excision and/or implementation of adjuvant therapy [13,23].
The subsequent “fulminant” recurrence with the patient’s death was a very humbling experience and supports the argument of aiming for a “100% level” as the target level of marginal excision. Immediate reconstruction or further delay of reconstruction probably would not have changed the fatal course of the disease resulting from the very unexpected change in the tumor’s aggressiveness. However, perhaps a more detailed characterization of the histology of the tumor, tumor grade, molecular markers associated with a more malignant course, and neoadjuvant treatment, would lead to a change in ablative strategy, resulting in a more extensive resection or even an amputative approach and the utilization of an immediate flap based reconstruction with brachytherapy would conceivably improve the outcome [14,16,17]. This case of a liposarcoma and this type of case management could hypothetically be used and implemented to reaffirm the opinion that the analysis of the outcomes versus the recommendations for immediate or delayed reconstruction should be very individualized, or that determining standard procedures for the decision must involve very large groups of patients with homogenous conditions [7,22]. Indirectly and in retrospect, this case answers the emerging question whether there are scenarios when immediate reconstruction – as opposed to delayed reconstruction - could positively impact the final outcome regardless of the CDP score [13,18].
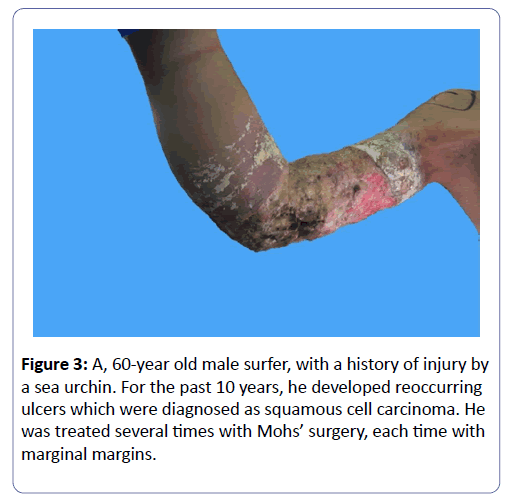
Similarly, in a case of an advanced squamous cell carcinoma of the entire upper extremity and the axilla, the histological mapping of the proximal margin of amputates proved to be highly impractical intraoperatively (Figure 3). The patient had revisional amputation twice (for the removal of local metastases). In this case, immediate reconstruction would have been inappropriate [9,10].
These cases demonstrate that all CDPs should be known before the definitive reconstruction strategy is decided. These factors are not synonymous with prognostic factors although to a degree similar [4,26]. Since surgery remains the mainstay of extremity sarcoma and squamous cell carcinoma treatment, CDP scores may help in decisional practicalities such as to at what point in time to proceed with reconstruction, but not necessarily in deciding on different combinations of treatments or the scope of all treatments. Experience regarding the safety of margins in immediate versus delayed free tissue transfer for lower extremity salvage after surgery in cases of soft tissue sarcoma or squamous cell carcinoma, emphasizes the reliability and quality of surgical outcomes, the rate of wound complications, and faster rehabilitation. However, the data do not address outcomes in the context of long-term problems resulting from possible inadequate margins [1,7,28,29]. The timing of reconstructive surgery is frequently highlighted with the bias that immediate or early reconstruction achieves better results with lesser complication rates, however, these studies do not specify how post malignancy excision wounds were cared for in preparation for delayed intervention [4,28-30]. In the presented cohort, in order to avoid infections and subsequent complications in patients scheduled for delayed reconstruction, wounds were temporized with systems completely sealing the resected area (vacuum assisted wound closure devices or skin substitutes).
In addition to clinical experience regarding specific tumor entities, new imaging techniques may be useful in avoiding “one size fits all” management strategies, to determine safe margins and to evaluate the responses to auxiliary treatments (if there are any). 18F-fluorodeoxyglucose positron emission tomography/computed tomography has recently been introduced and presents as a helpful tool for the mapping of sarcoma affected tissues [4,7,24,25]. Modern precise three-dimensional tumor imaging techniques allow for the relatively effective implementation of curative resections, which are both appropriately extensive and selective at the same time. Modern imaging allows the adoption and utilization of surgical advantages provided by biological barriers of tumors (e.g., fascia, periosteum, cartilage). It also allows for the sparing of tissue which would have to be excised if one would follow extensive compartmental resections and may even allow for the use of some spared tissue for the reconstruction process [4,5,9,26,27].
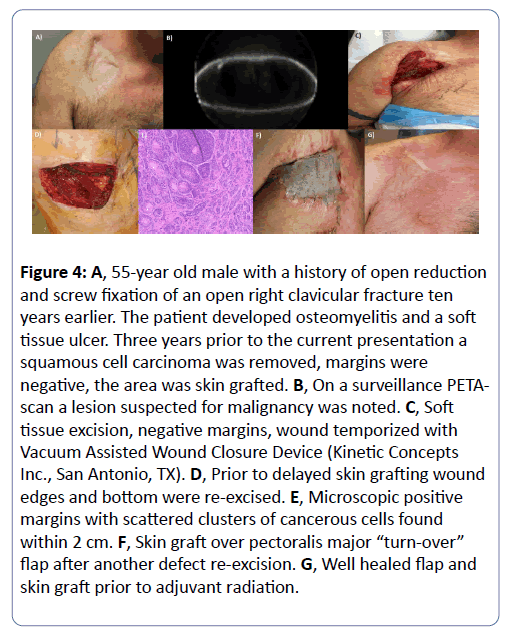
Regardless of the discussion of whether “absolute” local control impacts survival, probably no one would question that for the success of reconstructive surgery, it is imperative that the margins are safe and cleared of tumor [4,7,27,28]. Accurate assessment of the microscopic margins requires that the specimen is presented to a pathologist as a single intact tissue segment whenever possible. Specimen orientation and the documentation of orientation for the pathologist is of critical value in the event of a positive or close margin in the specimen, since this information can be used to direct further surgery [28-31]. Even when the field is prepared for reconstruction with margins previously declared “negative,” it is wise to submit any tissue removed in the process of reconstruction solely enabling reconstruction with orientation markings for the pathologist as sometimes there may be an unexpected finding (Figure 4).
Figure 4: A, 55-year old male with a history of open reduction and screw fixation of an open right clavicular fracture ten years earlier. The patient developed osteomyelitis and a soft tissue ulcer. Three years prior to the current presentation a squamous cell carcinoma was removed, margins were negative, the area was skin grafted. B, On a surveillance PETA-scan a lesion suspected for malignancy was noted. C, Soft tissue excision, negative margins, wound temporized with Vacuum Assisted Wound Closure Device (Kinetic Concepts Inc., San Antonio, TX). D, Prior to delayed skin grafting wound edges and bottom were re-excised. E, Microscopic positive margins with scattered clusters of cancerous cells found within 2 cm. F, Skin graft over pectoralis major “turn-over” flap after another defect re-excision. G, Well healed flap and skin graft prior to adjuvant radiation.
The presented analysis demonstrated multiple reasons for proceeding with the reconstruction at the right time, while this does not always involve an immediate intervention. One of the patients with a squamous cell carcinoma originating from a scar, exemplifies that one cannot always be 100% sure about the integrity of the margins, and that the non-appositional growth in poorly differentiated or high-risk tumors should always be considered prior to the reconstruction of soft tissues (this patient met 9 of 12 CDPs) (Figure 4). In retrospect, none of the courses of the diseases nor the outcomes of patient who received delayed reconstruction indicated that immediate reconstruction could have led to a more favorable result. One has to keep in mind that certain malignancies, for example Merkel cell carcinoma of the extremities, are known to be notorious for posing problems regarding the qualitative and quantitative adequacy of margins [28-30,32,33].
A growing extremity may pose a different type of reconstructive challenge. Other than assuring clean margins and a recurrence-free status, delay of definitive reconstruction may be done to give the extremity an opportunity to grow and develop (Figure 5). The same case, which was delayed for an extremely long period of time (4 years), underlines the importance of the techniques available to and used by plastic surgery for the temporization of a defect.
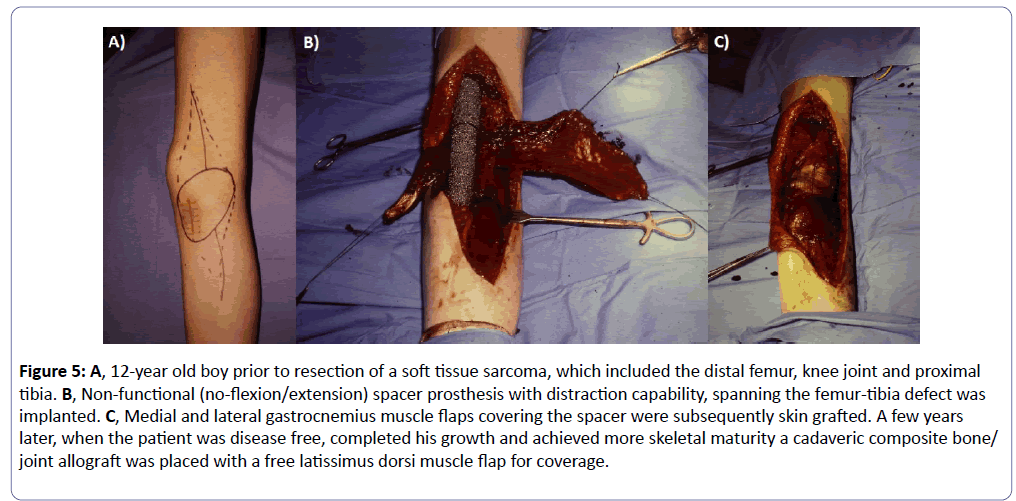
Figure 5: A, 12-year old boy prior to resection of a soft tissue sarcoma, which included the distal femur, knee joint and proximal tibia. B, Non-functional (no-flexion/extension) spacer prosthesis with distraction capability, spanning the femur-tibia defect was implanted. C, Medial and lateral gastrocnemius muscle flaps covering the spacer were subsequently skin grafted. A few years later, when the patient was disease free, completed his growth and achieved more skeletal maturity a cadaveric composite bone/ joint allograft was placed with a free latissimus dorsi muscle flap for coverage.
In general, the threshold, CDP or equivalent “numerical” approach for clinical decision making has the potential of improving patient quality of care. By identifying specific characteristics in which the ultimate reconstructive decision would not be affected by the specific factor, it could ultimately be possible to streamline and refine the list of factors to consider during the decision-making process [19]. Members of the Multidisciplinary Orthopedic team managing the extremity malignancies, expect some evidence based support for the recommendations of the reconstructive surgeon. For this reason alone, the development of a credible scoring system would be of great value. However, the author’s experiences related to the quantitation of CDPs is preliminary and, as discussed above, a threshold for the recommendation of when to proceed with delayed reconstruction has yet to be established.
Conclusion
Relative concordance between the decisions regarding immediate versus delayed definitive extremity reconstruction made at the time of pre-resectional planning or in the intraoperative setting, and those that were stipulated retrospectively when all information, including at the very least the short term outcomes, were at hand, reaffirms that an individualized, customized approach regarding the management of each patient and the assessment of the value of delayed definitive reconstruction in the given situation should be the modus operandi of the orthopedic-plastic surgery team treating advanced extremity malignancies.
References
- Chang EI, Nguyen AT, Hughes JK, Moeller J, Zhang H, et al. (2016) Optimization of free-flap limb salvage and maximizing function and quality of life following oncologic resection: 12-year experience. Ann Surg Oncol 23: 1036-1043.
- Mundiger GS, Prucz RB, Frassica FJ, Gene ED (2014) Concomitant upper extremity soft tissue sarcoma limb-sparing resection and functional reconstruction: assessment of outcomes and costs of surgery. Hand 9: 196-204.
- Reece GP, Schusterman MA, Pollock RE, Kroll SS, Miller MJ, et al.(1994) Immediate versus delayed free-tissue transfer salvage of the lower extremity in soft tissue sarcoma patients. Ann Surg Oncol 1: 11-17.
- Bonvalot S, Levy A, Terrier P, Tzanis D, Bellefqih S, et al. (2017) Primary extremity soft tissue sarcomas: does local control impact survival. AnnSurg Oncol 24: 194-201.
- Enneking WF, Spanier SS, Malawer MM (1981) The effect of anatomic setting on the results of surgical procedures for soft parts sarcoma of the thigh. Cancer 47: 1005-1022.
- Jones AP, Lewis CJ, Dildey P, Hide G, Ragbir M (2012) Lipoma or liposarcoma? A cautionary case report. J Plast Reconstr Aesth Surg 65: e11-e14.
- Katz SC (2017) Tailoring surgical therapy for extremity soft tissue sarcoma 24: 13-14.
- Randall RL, Bruckner JD, Papenhausen MD, Thurman T, Conrad EU (2004) Errors in diagnosis and margins determination of soft tissue sarcomas initially treated at non-tertiary centers. Orthopedics 27: 209-212.
- Trovik CS, Skjeldal S, Bauer H, Rydholm A, Jebsen N (2012) Reliability of margin assessment after surgery for extremity soft tissue sarcoma: The SSG experience. Sarcoma;18:epublication 290698.
- Jennings L, Schmults CD (2010) Management of high-risk cutaneous squamous cell carcinoma. J Clin Aesth Dermatol 3: 39-48.
- Keus RB, Rutgers EJT, Ho GH, Gortzak E, Albus-Lutter CE, et al. (1994) Limb-sparing therapy of extremity soft tissue sarcomas: treatment outcome and long term functional results. Eur J Cancer 30A: 1459-1463.
- Wang J, Shen J, Dickinson IC (2011) Functional outcome of arthrodesis with a vascularized fibular graft and a rotational latissimus dorsi flap after proximal humerus sarcoma resection. Ann Surg Oncol 18: 1852-1859.
- Gundle KR, Gupta S, Kafchinski L, Griffin AM, Kandel RA, et al. (2017) An analysis of tumor- and surgery-related factors that contribute to inadvertent positive margins following soft tissue sarcoma resection. Ann Surg Oncol 24: 2137-2144.
- McKnight AJ, Lewis VO, Rhines LD, Hanasono MM, et al. (2013) Femur-fibula-fillet of leg chimeric free flap for sacral-pelvic reconstruction. J Plast Reconstr Aesth Surg 66: 1784-1787.
- Samant M, Chang EI, Petrungaro J, Ver Halen JP, Yu P, et al. (2012) Reconstruction of massive oncologic defects following extremity amputation. Ann Plast Surg 68: 467-471.
- Saba SC, Shaterian A, Tokin C, Dobke MK, Wallace AM (2012) The pedicled myocutanoeus flap as a choice reconstructive technique for immediate adjuvant brachytherapy in sarcoma treatment. Curr Oncol 19: e491-e495.
- Wasif N, Tamurian RM, Christensen S, Do L, Martinez SR (2012) Influence of specialty and clinical experience on treatment sequencing in multimodal management of soft tissue extremity sarcoma. Ann Surg Oncol 19: 504-510.
- Austin PC (2011) An introduction to propensity score methods for reducing the effects of confounding in observational studies. Multivariate Behav Res 46: 399-424.
- Pauker SG, Kassirer JP (1980) The threshold approach to clinical decision making. N Engl J Med 302: 1109-1117.
- Hoven-Gondrie ML, Bastiaannet E, Ho VKY, van Leeuwen BL, Liefers GJ, et al. (2016) Worse survival in elderly patients with extremity soft-tissue sarcoma. Ann Surg Oncol 23: 2577-2585.
- Mussi CE, Daolio P, Cimino M, Giardina F, Sanctis RD, et al (2014) Atypical lipomatous tumors: should they be treated like other sarcoma or not? Surgical consideration from a bi-institutional experience. Ann Surg Oncol 21: 4090-4097.
- Misra A, Mistry N, Grimer R (2009) The management of soft tissue sarcoma. J Plast Reconstr Aesth Surg 62: 161-174.
- Boro A, Bauer D, Born W, Fuchs B (2016) Plasma levels of miRNA-155 as a powerful diagnostic marker for dedifferentiated liposarcoma. Am J Cancer Res 6: 544-552.
- Yokouchi M, Terahara M, Nagano S (2011) CT and 18FDG-positron emission tomography in soft tissue sarcoma. BMC Musculoskeletal Disorders 12: 166-175.
- Kawaguchi N (1984) Curative limb saving operation (curative wide resection). Gan To Kagaku Ryoho 11: 1736-1745.
- Sanfilippo R, Miceli R, Grosso F, Fiore M, Puma E (2011) Myxofibrosarcoma: prognostic factors and survival in a series of patients treated at a single institution. Ann Surg Oncol 18: 720-725.
- King DM, Hackbarth DA, Kirkpatrick A (2012) Extremity soft tissue sarcoma resections: how wide do you need to be? Clin Orthop Relat Res 470: 692-699.
- Reece GP, Schusterman MA, Pollock RE, Kroll SS, Miller MJ, et al. (1994) Immediate versus delayed free tissue transfer salvage of the lower extremity in soft tissue sarcoma patients. Ann Surg Oncol 1: 11-17.
- Sanniec KJ, Velazco CS, Bryant LA (2016) Immediate versus delayed sarcoma reconstruction: impact on outcomes. Sarcoma, article 7972318: 1-5.
- Marre D, Buendia J, Hontanilla B (2011) Complications following reconstruction of soft tissue sarcoma. Importance of early participation of the plastic surgeon. Ann Plast Surg 69: 73-78.
- Wong KC, Kumta SM, Chiu KH (2007) Precision tumor resection and reconstruction using image-guided computer navigation. J Bone Joint Surg (Br) 89B: 943-947.
- Biau DJ, Weiss KR, Bhumbra RS, Davidson D, Brown C (2013) Monitoring the adequacy of surgical margins after resection of bone and soft-tissue sarcoma. Ann Surg Oncol 20: 1858-1864.
- Soltani AM, Allan BJ, Best MJ, Panthaki ZJ, Thaller SR (2014) Merkel cell carcinoma of the hand and upper extremity: current trends and outcomes. J Plast Reconstr Aesth Surg 67: e71-e77.
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences